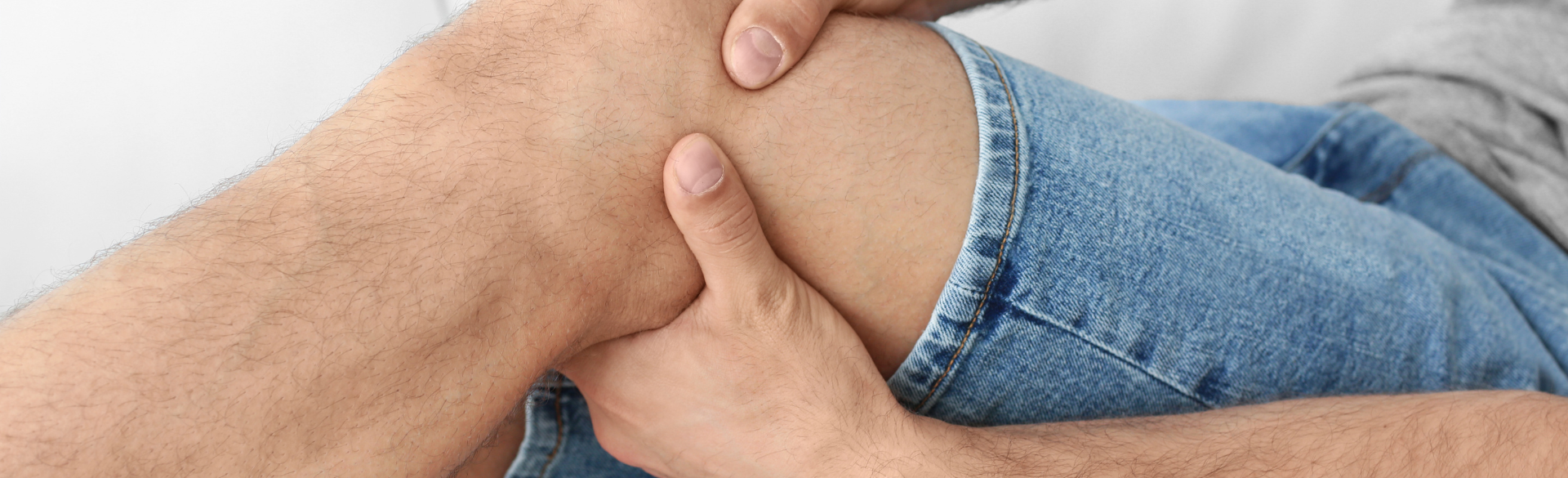
That pain when you walk could be more serious than you think. It could be a sign of peripheral artery disease (PAD), a condition in which a narrowing of the arteries results in reduced blood flow to the arms or legs. When the arms or legs — PAD typically affects the legs — don't receive enough blood flow to keep up with demand, it can cause pain when walking and other symptoms. PAD is usually a sign of a buildup of fatty deposits in the arteries, known as atherosclerosis.
September is PAD Awareness Month, a time to bring attention to the nearly 20 million Americans who are impacted by PAD, including an estimated 200,000 individuals who suffer preventable amputations every year due to complications from the chronic disease.
“One of the problems with peripheral artery disease is that people don't really know what it is or what it feels like,” says Marc Bonaca, MD, professor of cardiology at the University of Colorado School of Medicine. “People know what a heart attack or stroke is and what the symptoms are, but peripheral artery disease is underrecognized, and the risks associated with it are, are quite severe. The risk of having a heart attack or stroke or dying of cardiovascular causes even higher if you have PAD than if you have coronary disease or you've had a heart attack.”
Atherosclerosis is the most common cause of PAD, says Max Wohlauer, MD, associate professor of vascular surgery. Atherosclerosis is a hardening of the arteries due to a buildup of plaque. Atherosclerosis-related diseases are the leading cause of death in the United States. The main risk factor for PAD is cigarette smoking. “People can have genetic factors, but the typical risk factors are cigarette smoking, hyperlipidemia (elevated cholesterol or other lipids/fats), and high blood pressure. These things irritate the lining of the blood vessels,” he says. “The blood vessels harden, plaque builds up, and then the artery gets narrower. If it gets narrower to the point where it's slowing down blood flow, it can cause various symptoms, including pain when walking.”
Treatment gaps in patients with PAD
PAD is exacerbated by conditions like diabetes, chronic hypertension, and renal disease, which are most prevalent in minority populations. According to research from the Dartmouth Institute for Health Policy and Clinical Practice, African American, Hispanic, and Native American populations are two to four times more likely to undergo a limb amputation due to PAD because of the increased prevalence of diabetes, obesity, and other risk factors.
“At the CU Department of Surgery, we are working on reaching out to underserved communities about prevention and detection of this potentially dangerous condition,” Wohlauer explains.
Higher risk for other conditions
As PAD can indicate a narrowing of the arteries throughout the body, those who have it are at higher risk for stroke, heart attack, and kidney disease, Wohlauer says.
“That’s why it's really important to recognize it,” he says. “Screening for it is really important, because in the early stages, especially for asymptomatic PAD, medical treatment and risk factor modification makes a big difference.”
In addition to its trademark symptoms, PAD is detected by a test called an ankle-brachial index, which compares the blood pressure in the foot or ankle to the blood pressure in the arm. A low ankle-brachial index number can indicate narrowing or blockage of the arteries in the legs.
Symptoms and treatment
If someone with PAD does start to experience the primary symptom of pain and cramping when they walk, there is a supervised walking program that can help to include blood flow. Other treatments include medication and surgery.
Other symptoms of PAD include:
- Leg numbness or weakness.
- Skin color changes on the legs.
- Pain when using the arms, such as aching and cramping when knitting, writing, or doing other manual tasks.
- No pulse or a weak pulse in the legs or feet.
- Sores on the toes, feet, or legs that won't heal.
- Painful cramping in one or both of the hips, thighs, or calf muscles after certain activities, such as walking or climbing stairs.
- Coldness in the lower leg or foot, especially when compared with the other side.
- Hair loss or slower hair growth on the legs.
- Shiny skin on the legs.
- Slower growth of the toenails.
- Erectile dysfunction.
Some people with PAD have pain when they are lying down. If hanging the legs over the edge of the bed or walking relieves the pain temporarily, that’s a strong sign they have PAD.
“If you have pain when you walk, it’s important to understand whether your pain is related to peripheral artery disease, or something else,” Wohlauer says. “This is especially important if you have risk factors for PAD, or are concerned about PAD.”
Bonaca adds: “It’s also important to take care of your feet, as a black spot on the foot that won’t heal could be a sign of PAD.”
“The other important thing is to think about your older family members,” he says. “It could be your grandmother or grandfather, and they may not be aware of PAD but they have symptoms or may be slowing down. You can tell them, ‘Maybe it's your circulation; maybe you should talk to your doctor about it and get tested.’”
If you think you may have peripheral artery disease, please talk to your primary care provider about a referral to a vascular specialist.