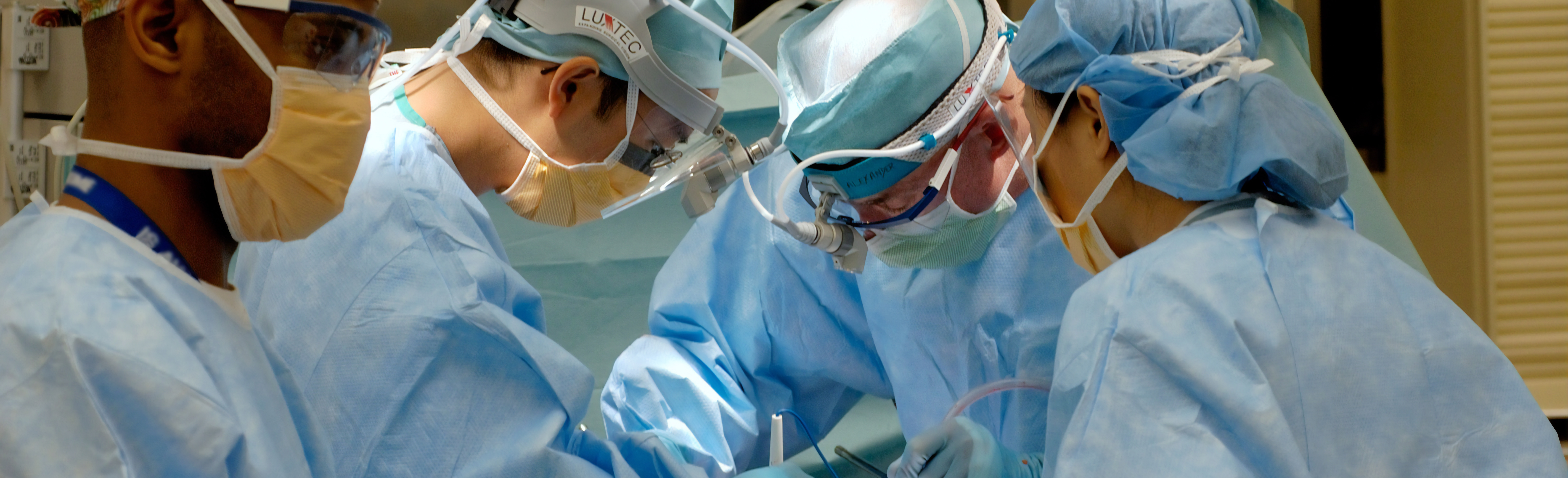
Carotid artery blowout, while rare, is a life-threatening surgical emergency with a mortality rate approaching 60%.
For the surgical team caring for a 37-year-old kidney-pancreas transplant patient who experienced carotid blowout (CB), this unexpected and extremely serious medical event highlighted the importance of prompt recognition and swift surgical treatment for CB.
In a recently published case study detailing the man’s CB, Ali Hakimi, a fourth-year medical student in the University of Colorado School of Medicine, and Jeniann Yi, MD, an assistant professor of vascular surgery in the CU Department of Surgery, outline this unexpected outcome for a patient with no known history of neck surgery or instrumentation.
“One of the reasons for publishing this case history is that it was such a rare and unanticipated outcome, which is really interesting from a surgical perspective,” Yi explains. “It’s also a reminder that transplant patients may have certain vulnerabilities, so it’s important to be vigilant and learn to recognize symptoms, even for something as rare as this.”
Concern about infection
The 37-year-old male patient, who has a history of hypertension and type 1 diabetes, received a combined kidney-pancreas transplant a year and a half before experiencing CB. In the four days before going to the emergency room, he had abdominal pain, nausea, vomiting, and diarrhea.
He was admitted to the hospital because the medical team caring for him was concerned about cytomegalovirus viremia (CMV) infection as well as acute hepatitis. On the sixth day of his hospitalization, despite improvement in the CMV, he developed sudden swelling and pain in the left side of his neck.
“Because of his transplant status, he was chronically immunosuppressed, which could make him more susceptible to getting an infection,” Hakimi explains. “He originally presented with a viral infection commonly seen in people with transplants.”
The medical team didn’t immediately think CB because “it just doesn’t happen that someone spontaneously bleeds from the carotid artery without reason,” Yi says. “Usually, the reason is traumatic – there was a central line being placed, for example, and it got into the carotid – or it can be secondary to other reasons that cause damage to the carotid artery, like radiation therapy for head and neck cancers or an infection.”
However, because of the swelling, his care team scanned his neck and found the carotid artery bleeding, which is when Yi and the vascular surgery team were brought in to provide treatment.
Treating transplant patients
After beginning surgery, Yi saw that his carotid artery had a lot of inflammation and “looked like it was chewed up, like something had degraded it, which is what it would look like in the setting of infection,” she says. “Primary infection of an artery anywhere is bizarre. In general, it’s hard for an artery to be infected because there’s such high blood flow that there’s not enough contact time. We never could find a great reason why it happened, so we had to assume it was an infectious reason based off his history and based off what it looked like in the OR.”
Yi performed a bypass, removing the part of his carotid artery that was violated by the suspected infection and then using his vein for the bypass.
“A bypass is as good a repair as you can get,” she says. “It’s the most infection-resistant repair because a vein is his own native tissue with the least amount of infectious possibility. A graft or a stent could get infected.”
Through performing a literature review, Hakimi learned just how rare-to-nonexistent CB is in this circumstance “so the best we could do was theorize that there’s a link between CMV and the carotid – there’s something about that tissue that CMV is more likely to affect or seed it,” he explains.
This case could inspire further research at the intersection of transplant and immunosuppression, Yi says, as well as help educate health care providers who treat transplant patients.
“It’s a reminder that anything can happen with chronic immunosuppression like in transplant patients, including spontaneous infection of an artery and a ruptured pseudo-aneurysm,” Yi says. “Considering everything I’ve ever experienced as a vascular surgeon, this is not something I could think about as being a potential complication, but now it’s something I’m aware of.”