When the PACT Act went into effect January 1, after being signed into law in August, many U.S. veterans were able to access benefits for an expanded list of health conditions presumed to be caused by exposure to toxic substances.
These exposures include airborne hazards resulting from burn pits, and among the conditions presumed to be a result of military service are many types of cancer. Under the PACT Act, now any type of head cancer and any type of neck cancer are considered presumptive, as well as several other types of cancer.
April is Head and Neck Cancer Awareness Month, an important time to not only highlight this group of cancers, but the impact they are having on veteran populations.
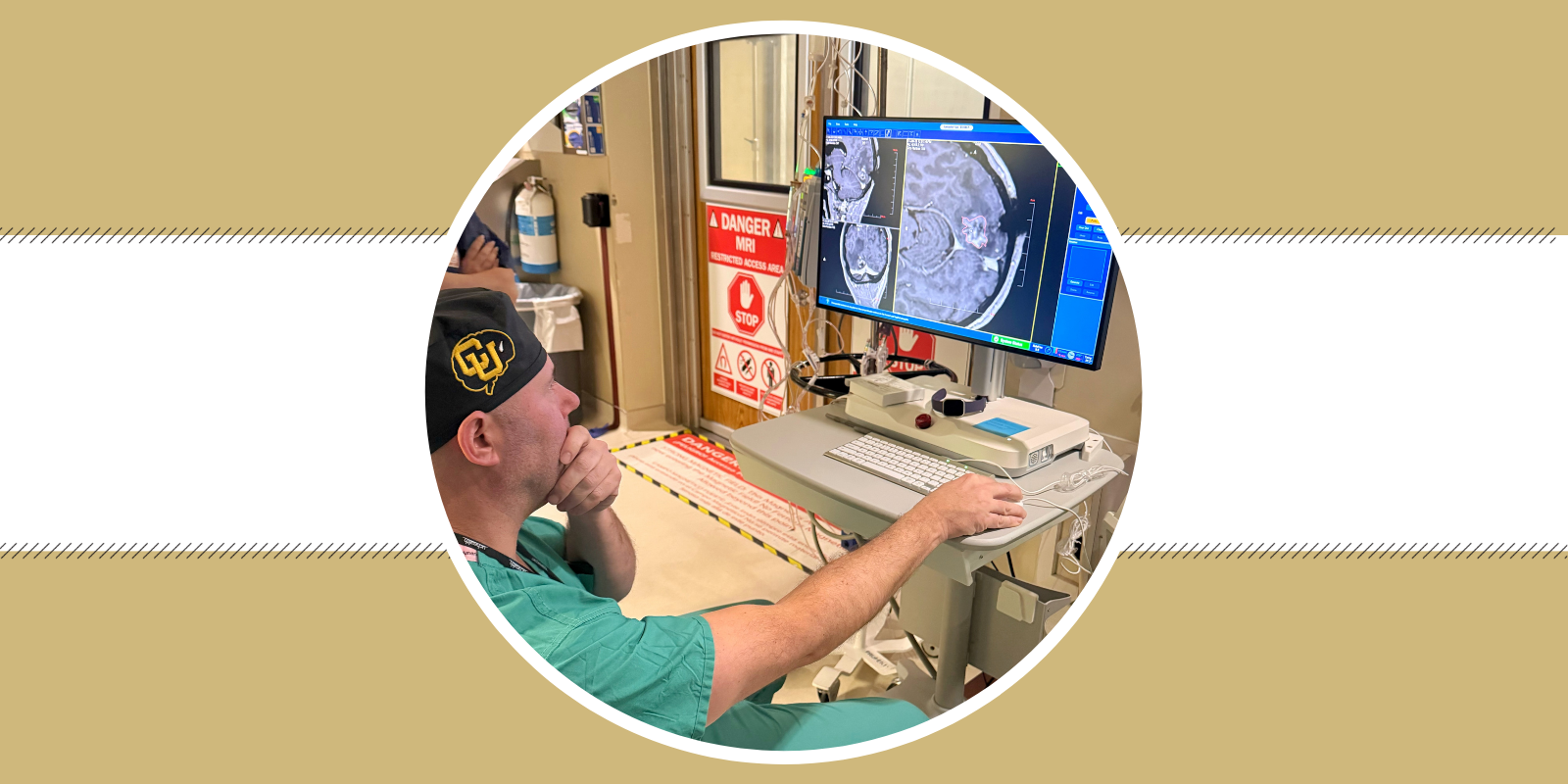
“We’re definitely seeing younger veterans with some of these head and neck cancers that you would typically expect to see in older patients, or we’re seeing veterans with multiple different cancers at once and they often seem presumptively related to these exposures,” says Jessica McDermott, MD, deputy associate director of diversity and inclusion in clinical research in the University of Colorado Cancer Center.
PACT Act expansions
The Sergeant First Class (SFC) Heath Robinson Honoring our Promise to Address Comprehensive Toxics (PACT) Act greatly expanded Veterans Administration (VA) benefits for veterans who experienced toxic exposures in Vietnam, the Gulf War, and post-9/11 eras. The PACT Act requires the VA to provide a toxic exposure screening to every veteran enrolled in VA health care, and adds more than 20 presumptive conditions for burn pits, Agent Orange, and other toxic exposures.
“A question we get fairly regularly is what it means to have a presumptive condition for a toxic exposure,” says McDermott, an assistant professor of medical oncology in the CU School of medicine whose practice includes the Rocky Mountain Regional Veterans Administration Medical Center. “For some of the conditions that are now covered under the PACT Act, a patient and their provider would have to prove that their military service caused the condition, and for a lot of cancers direct causation can be very difficult to prove.
“Under PACT, for the conditions it covers, it’s now automatically assumed that a veteran’s military service led to the condition. It’s still not uncommon for our patients to think they have to prove somehow that they served in a particular area for a certain amount of time, and they breathed this amount of airborne toxins. But now we have it nicely laid out that if they served in certain areas during certain times, this expanded list of conditions is presumed to have been caused by their service and those exposures.”
Understanding exposures
The head and neck cancers included in the expanded list of presumptive conditions are important for many reasons, including the fact that there often is less awareness of these cancers, McDermott says.
“People will first associate lung cancer with breathing in exposures, but when you’re inhaling something it has to bypass the nose, the thyroid, the larynx, the oropharynx and they’re all at risk for exposures,” McDermott explains. “Head and neck cancers do have quite a few overlapping risk factors with lung cancer, but I think the general public just tends to know less about them.”
She adds that the average age for presentation with head and neck cancers is late 50s to 60s, but that she and her colleagues are seeing some younger veterans presenting with them, and sometimes at more advanced stages of disease.
While there are many factors that can influence a head and neck cancer diagnosis – including smoking history, access to medical care, and exposure to human papillomavirus, among many others – burn pit exposures are presenting a growing challenge for patients, clinicians, and researchers.
“A lot of these exposures happened in our most recent wars, in Iraq and Afghanistan, so we’re really trying to catch in up in terms of what we know about risk and outcomes,” McDermott says, adding that the medical community as a whole is working to grow awareness in veteran populations of symptoms to be aware of related to head and neck as well as other cancers.
“For veterans or anybody else, if you have any unexplained neck nodules or neck nodes, any trouble swallowing, any new hoarseness that doesn’t go away, any unexplained weight loss, all those are things to pay attention to,” McDermott says. “We don’t have great screening right now for head and neck cancers, so that awareness piece is key.
“Veteran populations sometimes are not accessing dental care as consistently, and oftentimes dentists are catching certain head and neck cancers, so I think we need to be supporting our veterans in getting regular dental care, as well as having regular access to primary care. If they’re feeling that something isn’t right, or even if they know they had a burn pit exposure and want to ask about it, it’s important that we’re supporting them to get signed up for VA care and access their benefits.”