Editor’s note: “Our COVID-19 Fighters” is an occasional series highlighting the ways the CU Anschutz Medical Campus community is helping patients and the wider community in the fight against the pandemic. We welcome your story ideas; please share them here.
Using a high-quality antibody test produced within their own walls, researchers at the Barbara Davis Center for Diabetes (BDC) aim to answer questions about COVID-19’s effect on their patients – including whether SARS-CoV-2 can trigger one of the nation’s top chronic diseases.
The antibody test, created in the lab of Liping Yu, MD, was added this month to the Autoimmunity Screening for Kids (ASK) Program at the University of Colorado Anschutz Medical Campus. Open to all Colorado youth under 18, the ASK Program offers type 1 diabetes and celiac disease screenings. Parents now can also opt to have their kids tested for COVID-19 antibodies.
“And the best part of it is, it’s free,” said BDC Executive Director Marian Rewers, MD, PhD, adding that a COVID-19 antibody test alone generally runs about $100.
Part of the CU School of Medicine, the premier Barbara Davis Center conducts research and provides care to more than 7,500 patients across the region, with a prime focus on children and teens with type 1 diabetes. A disturbing trend within its type 1 patient population prompted the study.
‘This year was different’
New type 1 diagnoses generally follow a seasonal pattern, dropping dramatically in the late-spring and summer months, Rewers said. “This year was different.” After the pandemic began taking hold, BDC saw a 40% increase in new-onset pediatric cases in May and June compared with the same time period in 2019.
“Maybe it’s the straw that breaks the camel’s back.”
– Dr. Marian Rewers on COVID-19 infection
“It’s an indirect clue that the infection may actually precipitate high blood sugars,” Rewers said. “Maybe it’s the straw that breaks the camel’s back.”
In people with type 1 diabetes, insulin-producing beta cells (needed to convert blood sugar to energy) are destroyed. When not enough beta cells remain to do the job, generally in childhood, onset of the disease occurs. Patients then require insulin injections for life to maintain blood-sugar (glucose) balance.
Experts suspect ACE2 receptors expressed on the beta cells in the pancreas open the door for COVID-19 destruction, possibly triggering the onset of the disease in patients sooner. SARS-CoV-2 causes damage by binding to ACE2 receptors once inside the body and then entering the cells, wreaking its havoc wherever the virus lands, largely in the lungs, brain and gastrointestinal tract, Rewers said.
Big problem, old theory
A suspected 88 million Americans have pre-diabetes, most of them unknowingly. The vast majority of the 34 million-plus diabetes cases (a number that has doubled in the past 20 years) are type 2, with type 1 constituting 5% to 10% of cases. Based on ASK screening data, an estimated 700,000 U.S. children have pre-type 1 diabetes.
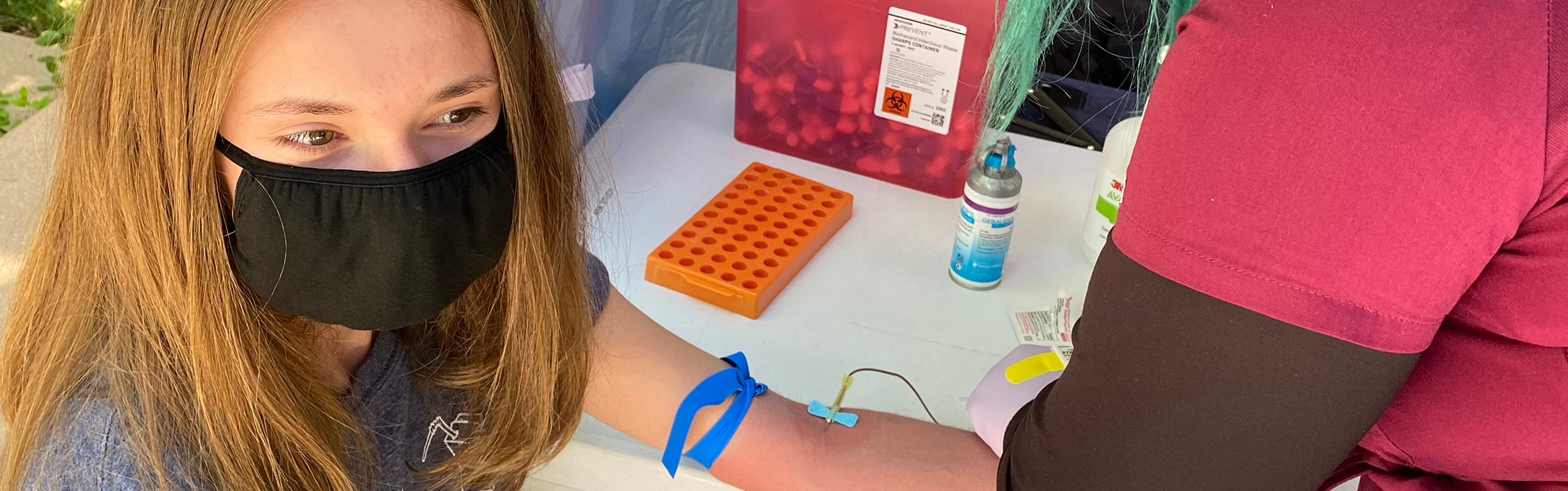 Professional Research Assistant Maria Saucedo collects a blood sample that will be tested for both COVID-19 antibodies and type 1 diabetes autoantibodies.
Professional Research Assistant Maria Saucedo collects a blood sample that will be tested for both COVID-19 antibodies and type 1 diabetes autoantibodies.
“So it’s a big problem, because we have a lot of people with pre-diabetes, and it looks like it doesn’t take a lot to push them over the brink to clinical diabetes,” Rewers said.
Although the study will focus only on type 1 disease, the work can inform wider diabetes studies. While type 1 and 2 diabetes have significant differences, they share the same “battleground” – a pancreas armed with crippled beta cells, Rewers said.
“When you look at the literature, although still very limited, what’s been published about coronavirus and diabetes and the effect on beta cells seems very similar for type 1 and type 2,” he said, noting that patients also have emerged from COVID-19 infections with type 2 diabetes.
The theory that SARS-CoV-2 could spark type 1 diabetes onset is not unprecedented. “We know that specific viruses can start the process and make kids progress faster to diabetes,” Rewers said.
Published December 2019 in Nature Medicine, The Environmental Determinants of Diabetes in the Young (TEDDY) study Rewers is leading found strong evidence that enteroviruses and adenoviruses can enter and kill beta cells, using a different receptor called CAR.
Bottom line: better care
The new study’s chief aim will be to determine if children positive for both type 1 autoantibodies and SARS-CoV-2 antibodies will progress faster to clinical diabetes than their counterparts with type 1 autoantibodies but no SARS-CoV-2 antibodies. ASK screens about 100 to 150 patients a week, so the research should also offer a glimpse into the prevalence of COVID-19 in the community.
Parents can opt out of the COVID-19 antibody test and still have their children screened for the autoimmune diseases. The center also intends to offer the test to ASK patients’ parents in the coming weeks.
 Dr. Luping Yu's research lab in the Barbara Davis Center for Diabetes recently developed its own COVID-19 antibody test.
Dr. Luping Yu's research lab in the Barbara Davis Center for Diabetes recently developed its own COVID-19 antibody test.
Experts believe COVID-19 antibodies can be detected in blood for nine months or longer post-infection, Rewers said. CLIA (Clinical Laboratory Improvement Amendments) validation of the Yu lab antibody test indicated that it is 100% sensitive (each sample tested of 70 patients with laboratory confirmed COVID-19 infection was positive) and 99.9% specific (one false positive arose from 1,006 pre-September 2019 blood samples).
“So this is a very good test,” Rewers said. “Dr. Yu is already running all of the tests the ASK study uses to find kids with early type 1 diabetes or celiac disease, so it’s the same blood sample, same lab, very easy and convenient,” Rewers said.
Should researchers confirm their theories, preventive care, education and treatments could help break the trends, such as ensuring those with, or at higher risk for, diabetes get vaccines first when that day comes, Rewers said. “We can help protect our kids who don’t have diabetes yet and patients who already have the disease. That’s what we do.”
Facts from the Autoimmunity Screening for Kids (ASK) Program:
- Launched in 2017, ASK provides free testing to Colorado children for type 1 diabetes and celiac disease autoantibodies.
- So far, ASK has screened more than 25,000 Coloradans under age 18 for the two most-common autoimmune disorders, affecting 1 in 30 children.
- When autoantibody markers are detected, those children are monitored and their parents educated in order to keep complications at bay.
- Of 25 children who progressed to diabetes while being monitored by ASK, only one needed to be hospitalized. In contrast, more than 60% of newly diagnosed children who did not participate in ASK had to be hospitalized at their diagnosis.
- Of children diagnosed with the disease, 90% have no family history of diabetes.
- Recent BDC research found 67% of Colorado kids present in the hospital with potentially fatal diabetic ketoacidosis (DKA) at disease onset.
- Detecting type 1 diabetes risk in children before its onset can make a significant difference in those children’s health for their lifespans, especially if DKA episodes are prevented.
- Research shows that DKA at onset significantly reduces lifelong success with managing the disease, with each subsequent DKA episode further complicating management.
Photo at top: Cristy Geno Rasmussen, program director for the ASK Program, poses with her kids after having them tested at the outdoor screening site.
Check out the story featured on 9News: Q&A: Can the coronavirus trigger type 1 diabetes in kids?



