At first glance, dry eyes may seem like a minor complaint, but eye care providers at the Sue Anschutz-Rodgers Eye Center on the University of Colorado Anschutz Medical Campus know that severe cases can be difficult to treat, often stemming from multiple factors. Left untreated, dry eye disease can impair vision and affect quality of life.
In September, the eye center began offering a relatively new treatment – intense pulsed light therapy (IPL) – where gentle pulses of light are used to treat the underlying causes of dry eye. For dry eye specialist Scott Hauswirth, OD, director of the CU Department of Ophthalmology’s Ocular Surface Clinic and assistant professor of ophthalmology at the CU School of Medicine, it’s been gratifying to have another therapeutic tool for dry eye disease.
“I have several years of experience working with the technology and was excited to bring it to the university,” he says. “Some of the initial papers reporting its efficacy in treating patients with dry eye were from clinicians I worked with. Patients were very pleased with what it could do for them, and it has continued to garner more supportive research. Its utilization worldwide has grown.”
Darren Gregory, MD, world-renowned expert in ocular surface disease and associate professor of ophthalmology at the CU School of Medicine, along with other corneal surgeons at the Sue Anschutz-Rodgers Eye Center will also be available to provide IPL treatment to patients.
 A patient receives intense pulsed light (IPL) therapy at the Sue Anschutz-Rodgers Eye Center.
A patient receives intense pulsed light (IPL) therapy at the Sue Anschutz-Rodgers Eye Center.
The evolution of IPL treatment
For decades, dermatologists used IPL for a variety of purposes such as hair removal and treating vascular lesions. When they began treating rosacea, a skin condition that causes blushing, with IPL in the early 2000s, a beneficial side effect emerged: some patients reported their dry eyes were alleviated after the procedure. In 2021, the Food and Drug Administration approved an IPL device labeled specifically for dry eye treatment.
IPL technology is particularly effective in targeting dry eyes caused by meibomian gland dysfunction, especially when there is associated inflammation of the adjacent skin. The meibomian glands produce the oil component of tears and help keep the surface of the eye moist.
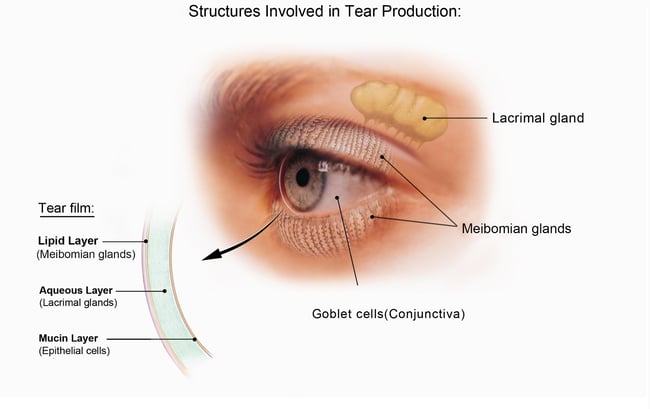
IPL therapy is meant to address dry eyes caused by meibomian gland dysfunction. Meibomian glands produce an oil found in tears.
Image courtesy of the National Eye Institute.
“Several studies show decreases in inflammatory levels in the tear film following treatment, as well as improved tear film stability and improved oil gland function,” Hauswirth says.
Application in ophthalmology
IPL is typically used when dry eye disease persists after a patient has tried first-line treatments such as prescription eye drops. During the procedure, patients are fitted with special goggles or shields to protect their eyes and ultrasound gel is applied to the surrounding areas. It is not painful and patients can see well immediately following the procedure.
The IPL device is about the size of a handheld grocery store price scanner. During the appointment, the device is moved across the skin of the cheeks and emits very short bursts of light energy. It is common to feel a small “tap” or “snap” from the light, almost like a small rubber band was released onto the skin. Afterwards, the treated area will feel warm, similar to a mild sunburn. The treatment takes about 10 to 15 minutes and is generally given in three to four treatments over the span of about three months.
“In my experience it usually takes about two treatments for the patient to notice improvement in their eyes, and severe cases may take longer,” Hauswirth says.
The treatment is not advisable for people with dark skin tones, as the light energy is absorbed more intensely and may cause loss of pigment or even cause burns to the skin.
Although it’s only been a month since the CU Department of Ophthalmology faculty began offering the treatments, Hauswirth is optimistic about having another option to offer patients.
“Dry eye can be a difficult disease to treat as many patients require therapeutic packages customized to address their root problem,” he says. “It is great to be able to customize treatment further with the addition of IPL to our arsenal.”
.png)
.png)
.png)

.png)
.png)