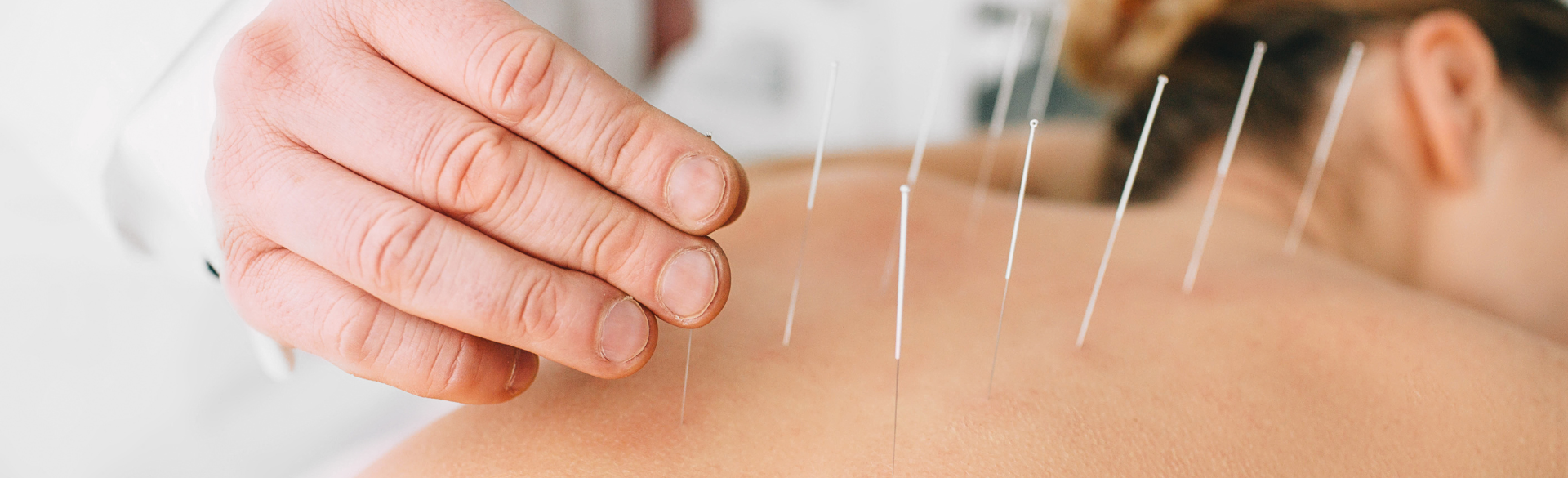
Yoga, massage, and bright white light therapy are among the effective ways to manage cancer-related fatigue, according to new patient guidelines from the National Comprehensive Cancer Network (NCCN).
The fatigue guidelines — which were given final review by University of Colorado Cancer Center member Catherine Jankowski, PhD, chair of the NCCN Panel for Cancer-Related Fatigue — were released in October along with new patient guidelines on palliative care and updated information on managing distress during cancer care. The CU Cancer Center is a member of NCCN, a not-for-profit alliance of 32 leading cancer centers devoted to patient care, research, and education.
“This is the first time the NCCN has issued patient-facing cancer-related fatigue and quality-of-life guidelines,” says Jankowski, professor in the CU College of Nursing. “It gives the patient the confidence that what they’re seeing in the guidelines is not new to their provider, and perhaps it gives them some confidence in asking for alternative fatigue therapies, whether that’s yoga, massage, or acupuncture.”
The patient-facing guidelines were released concurrently with the NCCN’s latest provider-facing guidelines for cancer-related fatigue, which are updated every year. Jankowski oversees the updating process for the provider-facing guidelines, which, like the patient-facing guidance, are evidence-based, citing the latest data and studies on the topic.
Fatigue causes and treatment
Fatigue is a common side effect of cancer treatments, but it has other causes as well, Jankowski says, including the stress that goes along with a cancer diagnosis and living with the disease.
“It can be caused by the cancer itself, it can be treatment-related, it can be a combination of the cancer with other preexisting medical conditions,” she says. “It can also be from the stress of having cancer. For example, someone who is the primary wage-earner and has used up their medical leave may return to work before they’re physically ready; this can cause a lot of stress, which can also cause fatigue. It's bidirectional — fatigue can also be very distressing. We want to make sure that patients have a broad perspective and the best available information about how fatigue might be affecting them and what they can do about it.”
The new patient guidelines discuss several different treatments for cancer-related fatigue, including mild to moderate physical activity.
“There is consistently favorable evidence that physical activity helps to reduce fatigue,” Jankowski says. “It also prevents deconditioning, which in the long term can contribute to more fatigue and other health conditions. As we’re looking at the entire health of the person, physical activity affects many physiological systems and has many benefits.”
Increased focus on integrative therapies
Other recommended therapies for fatigue, based on the literature, include massage, acupuncture, yoga, and bright white light therapy, in which a patient is exposed to a therapeutic bright light for a set duration of time. The guidelines don’t include any information as far as frequency and duration, due to the variability among patients and their individual experiences.
“It would be up to the patient and the therapists they’re working with, based on the severity of their symptoms,” Jankowski says. “We also have to be aware of the fact that not all health insurance plans cover all supportive or integrative therapies. In all cancer survivorship, there’s also a financial burden, and we want to be aware of that.”
One of the hopes with the patient-facing, as well as the provider-facing guidelines, she says, is to raise awareness of integrative therapies such as massage and acupuncture so that insurance companies who don’t already cover them for people with cancer might be persuaded to do so.
“When health insurance panels are meeting and deciding what they’re going to cover, we want to advocate based on scientific evidence,” she says. “Our recommendations can be very influential in that regard. The more careful we are and the more conscientious we are about making our recommendations, the greater the hope is that some of these alternative types of therapies will be covered by insurance.”
Part of the journey
Jankowski notes that many cancer-related fatigue treatments recommended in the new guidelines — including bright white light therapy — are currently offered at the CU Cancer Center, and the BfitBwell exercise program for cancer survivors is offered at the CU Anschutz Health and Wellness Center. Patient navigators in the CU Cancer Center could be consulted to locate other treatment resources.
In addition to making survivors aware of the different treatment options for their fatigue, she also hopes the guidelines help patients to recognize fatigue as part of the cancer journey.
“We want patients and caregivers to be aware of the breadth of cancer-related fatigue and how it manifests,” she says. “It can be very individualized; it can occur at any time in the cancer survivorship journey. And it can be recurring. It can go away for a long time and come back, or it might spring up much later. We want to raise awareness of the very different profiles it can have.”