After nearly four years of work, a group of researchers and clinicians from the University of Colorado (CU) published a paper this week in the Clinical Cancer Research that shares findings from research looking at how the composition of ovarian cancer tumors changes during chemotherapy and contributes to therapeutic response.
While the standard of care consisting of surgery and chemotherapy for ovarian cancer patients is usually effective, disease recurrence and resistance are common. In fact, according to the American Cancer Society, ovarian cancer ranks fifth in cancer deaths among women, accounting for more deaths than any other cancer of the female reproductive system. In 2020 it is estimated that 13,940 women will die from ovarian cancer. There is currently an unmet clinical need to predict patients’ response to chemotherapy, which was the focus of the research team.
“Almost all patients initially respond, however, almost all patients will recur,” says Benjamin Bitler, PhD, CU Cancer Center member and corresponding author. “On the other hand, there is a small percentage of patients will never recur or remain in remission beyond five years. We are working to be able to better predict a patients’ response to chemotherapy.”
This group of researchers and clinicians set out in November 2016 to focus on identifying potential biomarkers or pathways to better predict how a patient’s tumor would respond to therapy. This information could change maintenance and surveillance and will take a step towards a precision medical approach for each patient.
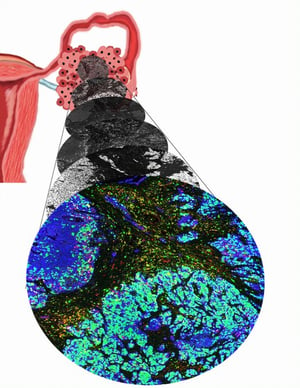
This image represents that multi-spectral immunohistochemistry
and the different cell populations.
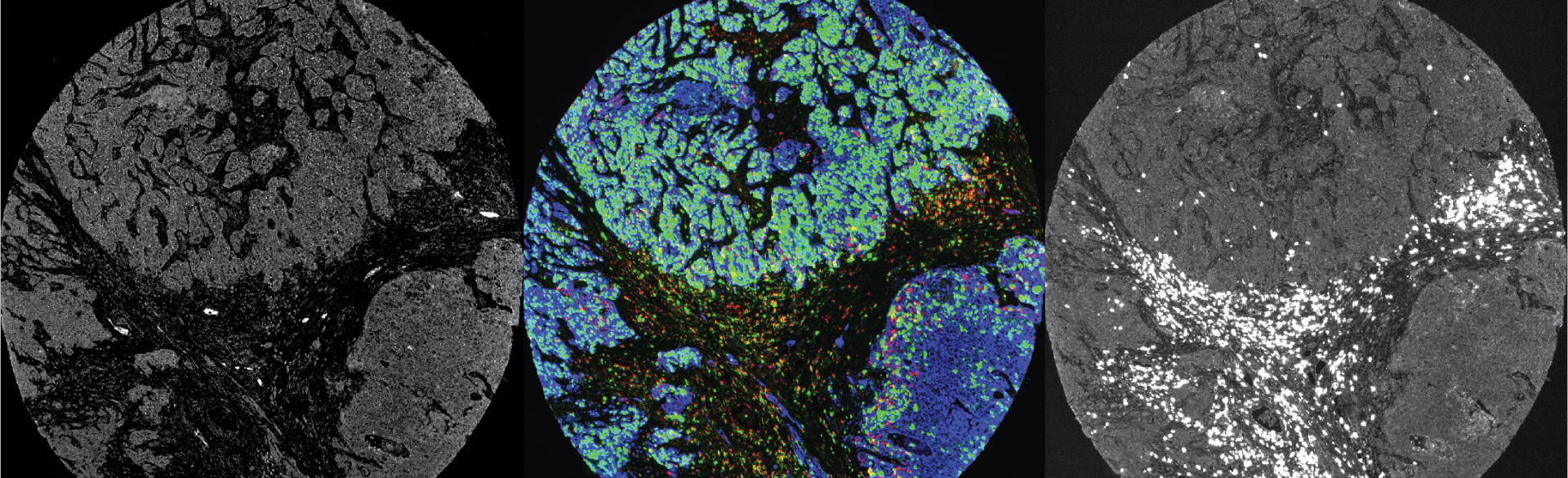
“Our ultimate goal is that someone who is diagnosed with ovarian cancer would be able to come in and we would be able to take the primary tumor and use the two major technologies described in the research study, transcriptomics using Nanostring and multi-spectral immunohistochemistry (IHC), to get an idea about what is being expressed and what the tumor microenvironment looks like,” says Bitler.
Multi-spectral IHC is a way of characterizing the tumor’s composition. Tumors are not made of only tumor cells; they also include among other things, blood vessels, stroma and immune cells. Other research leading up to this has shown the tumor composition correlates to the patient’s prognosis suggesting that the composition of the tumor likely holds clues as to therapeutic response. The major strength of multi-spectral IHC is that the location of the different cell types is kept intact, allowing for an added dimension of data, which is the physical location of each cell type.
“However, there is a limitation with multi-spectral IHC, which is that right now we can only identify nine different markers. This is a problem when you think there are likely more than 9 different subpopulations of cells within the tumor,” explains Bitler. “Therefore, to improve our resolution of the tumor composition we are using transcriptomic analysis in parallel to further infer into the tumor composition.”
Between these two technologies, the team can characterize the important players that might be involved in promoting the tumor progression or response to therapy. In the present study, the research group examined ovarian cancer tumors before and after chemotherapy, with the goal of describing how chemotherapy remodels the tumor composition. Building on this research study the long-term objective of the ovarian cancer research group to leverage our understanding of the effects of chemotherapy on the tumor to predict response and disease recurrence.
Looking forward in ovarian cancer care
One of the groups’ major funding sources to this point was an award through the Developmental Therapeutics program, one of four CU Cancer Center research programs.
“That award let us get to where we are right now but ultimately, we want to examine primary tumors from 500 patients.”
The team is getting ready to submit for a large federal grant later this year that will help with achieving our long-term goals. Dr. Aaron Clauset from CU Boulder is an expert in machine learning and network analysis. He will significantly contribute to aspects of the grant by developing machine learning approaches that predict therapeutic response.
“It is not going to happen in the next year or two but our long-term vision is that patients come in, get their tumor biopsied and within weeks we inform the clinician of the likelihood that his/her patient will be a good responder or be resistant to chemotherapy,” says Bitler.
Bringing two campuses together
“Another part of this project that I think is a strength, is that we were starting to bridge the gap between the CU Anschutz and CU Boulder campus to leverage the expertise, computer modeling and machine learning that is being developed in Boulder and apply it to some of the biomedical questions we have on the Anschutz campus,” says Bitler.
This study is made up of 15 researcher or clinicians, nine of which are CU Cancer Center members:
- Kimberly R. Jordan, PhD, co-first author, Department of Immunology and Microbiology.
- Matthew J. Sikora, PhD, co-first author, Department of Pathology.
- Jill E. Slansky, PhD, co-leader CU Cancer Tumor Host Interactions program, Department of Immunology and Microbiology.
- Angela Minic, MS, Department of Immunology and Microbiology.
- Jennifer K Richer, PhD, co-leader CU Cancer Tumor Host Interactions program, Department of Pathology.
- Marisa R. Moroney, MD, Department of OB/GYN, Division of Gynecologic Oncology.
- Junxiao Hu, MS, Department of Biostatistics and Informatics.
- Rebecca J. Wolsky, MD, Department of Pathology.
- Zachary L. Watson, PhD, Department of OB/GYN, Division of Reproductive Sciences.
- Tomomi M. Yamamoto, PhD, Department of OB/GYN, Division of Reproductive Sciences.
- James C. Costello, PhD, Department of Pharmacology.
- Aaron Clauset, PhD, Department of Computer Science.
- Kian Behbakht, MD, Lead clinician and Translational Scientist, Department of OB/GYN, Division of Gynecologic Oncology.
- Rajendra Kumar, PhD, Department of OB/GYN, Division of Reproductive Sciences.
- Benjamin G. Bitler, PhD, corresponding author, Department of OB/GYN, Division of Reproductive Sciences.
This group used a multidisciplinary approach to get to this point, which demonstrates the strength of putting the expertise of the two campuses together.
“This publication is a major milestone and a step in the right direction to show that we can work together as a team to address challenges that are facing patients with ovarian cancer.”
In addition to the project highlighted in this research study, The CU ovarian cancer research group also has on-going research projects. These projects include early detection of ovarian cancer (Dr. Behbakht; The Emily McClintock-Addlesperger Endowed Chair for ovarian cancer research), improving immunotherapeutic response (Drs. Richer, Slansky and Jordan), and uncovering new therapeutic targets (Drs. Sikora and Kumar).