There’s nothing new about people coming to hospital emergency departments for non-emergency reasons, and ED patient volumes have been rising for years. So far, it’s unclear whether those trends will be impacted by recent changes in federal policy – changes that are projected to increase the number of United States residents without health insurance by several million over the next few years.
The ED at UCHealth University of Colorado Hospital (UCH) is keeping an eye on the situation while it also plans for growing patient numbers, say two CU Anschutz Department of Emergency Medicine faculty members who work there.
“We are always looking ahead,” says Jean Hoffman, MD, associate professor of emergency medicine and medical director of the ED at UCH. “We’re always working on leveraging our entire health system to make sure that we're prepared for whatever is to come.”
“Every ED is talking about this,” says Gregory Adams, DO, an assistant professor of emergency medicine. “It’ll take time to see what the ramifications are going to be.”
Rising numbers
Nationwide, annual ED visits have been increasing for years as the population grows and ages, not counting a temporary decline during the COVID-19 pandemic. There were 155 million visits to U.S. EDs in 2022, according to federal data. The ED at UCH counted 127,682 visits in 2025.
Various U.S. studies have said a sizeable percentage of ED visits are for non-urgent purposes or for conditions treatable through primary care or at urgent-care facilities, but it's unclear precisely how often this happens. Many times, an ED visit can only be counted as non-urgent after physician assessment, Adams and Hoffman say.
Under the congressional 2025 Budget Reconciliation Act – also known as the One Big Beautiful Bill Act – signed into law in July 2025, federal Medicaid funding was reduced, many adults who receive Medicaid coverage must meet new work or training requirements starting in 2027, and some non-citizen immigrants are losing Medicare coverage.
Also, temporary federal tax credits for premiums to help lower-income people pay for health coverage through the Affordable Care Act marketplace, which were enacted during the COVID-19 pandemic, expired at the end of 2025. And ACA marketplace insurance premiums went up an average of 26% nationwide this year. (Colorado has enacted a premium assistance program for 2026 to help offset the loss of federal ACA premium credits.)
‘A big fear’
In July 2025, after Senate passage of the One Big Beautiful Bill, the American College of Emergency Physicians issued a statement saying: “The additional strain that this bill will impose by substantially increasing the number of uninsured or underinsured individuals will result in millions of patients with no other option to access care than the emergency department, further crowding already overburdened EDs, delaying care, and driving up costs for everyone.”
Nevertheless, a 2018 study drawing on national data found that uninsured adults were no more likely to use EDs than insured people. However, the uninsured group was less likely to seek health care from other kinds of providers. And according to federal data for 2022, people on Medicaid and Medicare visited EDs at higher rates than uninsured people, with people on private insurance visiting EDs at lower rates than other insurance-status groups.
Hoffman says that when the new federal health changes were passed, “there was a big fear that everyone was going to come running in because no one was going to have health care. So far, we have not seen people coming through our doors because of this legislation at any higher rate than before.”
Hoffman says the ED has always served “certain gaps of people who don’t have coverage. Usually, it’s those who make too much money to qualify for Medicaid, but they don’t get insurance through their job. And a lot of people are not citizens and are not eligible for many types of coverage.”
Many factors
At any rate, Hoffman and Adams say that insurance status is just one factor leading people to seek ED care for non-urgent needs instead of going to a primary care provider or an urgent-care facility. They include convenience and accessibility of EDs, difficulty accessing care elsewhere for various reasons, and limited knowledge of differences in care levels across settings and of the health care system in general.
Adams was a resident in Cleveland, including at a county hospital there. “Many of those patients didn't have access to care or a primary-care doctor, and didn't know how to navigate the system, so their safe move was to go to the ED,” he says. “I saw a lot of patients for things that I did not think needed an emergency department. That said, I knew they didn’t need an ED because this is my job. The average person might not be clear on what an urgent care or PCP can do for their acute concern.”
He also says that not all urgent-care centers provide the same services. “If you cut your hand on a kitchen knife and need stitches, some urgent cares can accomplish this while others can’t. It can be challenging for the average person to understand the capabilities of each facility. Sometimes the simplest answer is to go to the ED where there is more standardization of what can be treated.”
Adams also notes that some urgent-care centers may not accept all insurance plans, and often require a co-pay or deductible up front. “When a patient presents to an ED, they’ll be treated no matter their ability to pay,” he says.
He also mentions access-to-care hurdles. “Everyone knows where your ED is and you can come in 24/7, 365 days a year. For most primary care, generally you can’t just walk in, or they might be closed.”
Adams adds that what qualifies as urgent or non-urgent isn’t always clear at first. He recalls a patient he saw during residency who went to an urgent-care center, was diagnosed with acid reflux, and was sent home. “She was seen in our ED a few days later and we noted she’d suffered a heart attack. It can be challenging at times to make the distinction on certain patients and at times there is going to be a gray area.”
Hoffman says that even when patients head to an urgent care provider first, about 30% will wind up in the ED anyway.
Innovative intake
A surge in patients may pose less of a challenge at UCH’s ED than at many other emergency rooms because of its innovative patient intake system that eliminates triage, gets patients in front of a physician for evaluation in a few minutes, and aims to deliver care in 30 minutes or less for patients who don’t require additional testing. During peak times, patients with less serious conditions are moved to a “SuperTrack” team of nurses and advanced practice providers to speed their treatment.
“We keep things moving as efficiently as possible without ever sacrificing patient care,” Adams says.
The biggest challenge the UCH ED faces, Hoffman says, is “not someone who comes in with something that’s low acuity and who we can take care of quickly. The harder group is someone who expects something we can’t deliver. It might be someone who’s had a chronic complaint for several months – let’s say, knee pain for six months – and you need to access an MRI or a specialist. That’s really not what we were designed to do.”
Some patients see EDs as a more convenient option for care, Hoffman says. “People might say, ‘I want to see a specialist at 9 p.m. because I work during the day,’ or ‘I want to get all my work-up done in one place. I don’t want to have to make multiple appointments.’ People see us as a one-stop shop for expedited service. If you have an emergency, we are equipped to treat you, but we can not be everything in health care .”
As for concern about a potential surge caused by the unfolding federal policy changes, Hoffman says she and her colleagues “do a lot of projections, but we just don’t know yet what’s going to happen. Will we get higher volumes of lower-acuity patients? Will we get more higher-acuity patients because they don’t have insurance and don’t seek care? If we get both of those, that could be trouble. But in our hospital system, we are always planning for more volume and being operationally efficient.”
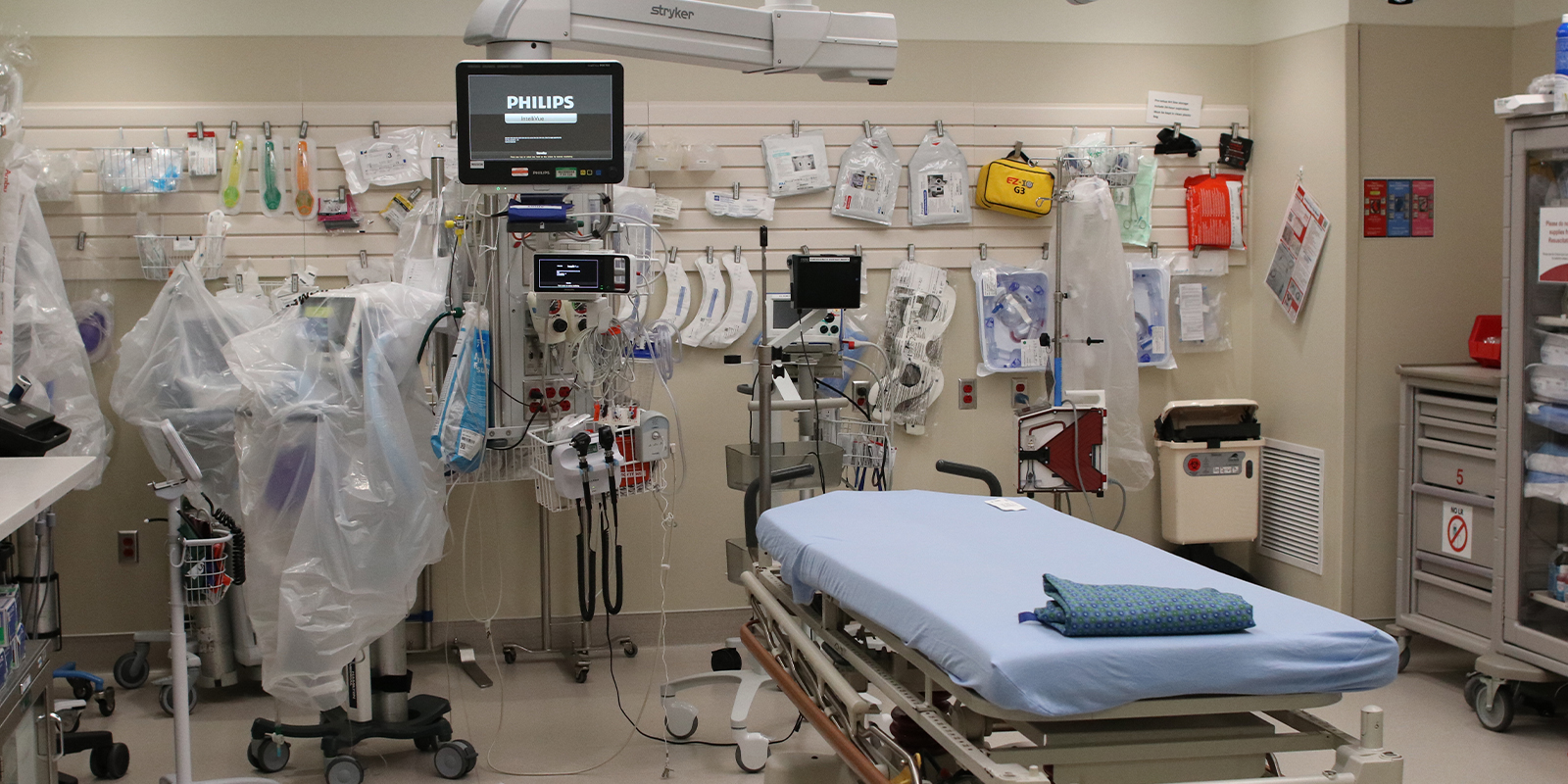
Photo at top: Treatment room in the UCHealth University of Colorado Hospital Emergency Department. Photo by Melissa Santorelli | University of Colorado School of Medicine