From the earliest days of the COVID-19 pandemic, communities of color have been hit hardest by the worst public health crisis in the past 100 years.
Black and Hispanic community members were more likely to contract the disease, more likely to be hospitalized because of it, and more likely to die due to its effects.
These grim statistics were driven by several factors: essential worker status, crowded housing and working conditions, reliance on public transportation, significant structural barriers to care, and a lack of accurate information about how to prevent exposure and protect against the virus, among others.
Seeing these challenges, University of Colorado School of Medicine faculty sprang to action to help those most in need.
Understanding the imbalance
Lilia Cervantes, MD, an associate professor in the Division of Hospital Medicine, quickly saw the impact of COVID-19.
While she was on the front lines, Cervantes began conducting research to understand the disproportionate burden Hispanic communities were facing and what interventions might help.
“They are often our essential workforce, and many of them don’t have the option to not work,” Cervantes says, “so they have to place themselves and their families at risk by taking public transportation and sometimes having to work despite being ill.”

Lilia Cervantes, MD, (center in black mask) talks with patient at a
vaccination clinic organized by Cynthia and Kweku Hazel.
Early in the pandemic, Cervantes interviewed 30 Hispanic patients who had been hospitalized for COVID-19 to understand the challenges these patients faced before going to the hospital, as well as their experiences in the hospital and after being discharged. Colleagues at the University of California, San Francisco, interviewed an additional 30 patients at their locations.
The research, published in JAMA Network Open, found that disease misinformation, financial pressures, and immigration concerns caused members of the Hispanic community to be at greater risk of exposure to COVID-19 and made them more likely to delay medical care. The study has led to local and national interventions to address these issues, including training staff at community-based organizations and offering pop-up vaccine clinics in medically underserved areas.
“It’s an important way to conduct research and effect change, which is to center the people who are marginalized and ask them to take the lead in creating strategies and solutions to mitigate the problem,” Cervantes says.
Community outreach and education
Long before the pandemic, husband-and-wife duo Kweku Hazel, MD, and Cynthia Hazel, DrPH, had already been conducting health-focused educational outreach, particularly within local Black communities.
“We were talking about hypertension, diabetes, obesity, cancer — all of these diseases that were ravaging our communities,” says Kweku, a clinical faculty/fellow in the CU Department of Surgery. “Once the pandemic hit, we had people reaching out and asking us to explain what was going on and help them navigate all the information they were receiving.”

Cynthia Hazel, DrPH, and Kweku Hazel, MD, (third and fourth from the left)
were joined by other volunteers at a vaccination clinic.
Because of the pandemic, in-person town halls moved to remote Zoom meetings and phone calls, but the format remained the same: panels and forums moderated by community leaders. The Hazels say their success relied on relationships they had already established with community leaders.
“We don’t know every community that’s interested in hearing from us, so the model we have used is to create community ambassadors and leave the organization to them,” says Cynthia, a public health research manager at the nonprofit OMNI Institute who graduated from the Colorado School of Public Health. “That’s part of how we’ve been able to build trust and relationships.”
“A lot of these groups already had established ways of keeping in touch, even during the pandemic, so that’s what we tapped into,” Kweku adds.
Shifting focus to vaccine shots
When the first vaccines started rolling out in the U.S. at the end of 2020, the Hazels’ emphasis shifted to how to best deliver them to underserved communities.
“When the vaccines started becoming available, it was assumed that the communities with the biggest share of COVID burden would be the most interested in getting vaccinated,” Cynthia says. “When that didn’t happen, it became clear that many of the same reasons these communities had a disproportionate burden of COVID also created barriers for them to get vaccinated.”
Although she and Kweku were available to address concerns about the science of the vaccine or religious issues, it wasn’t only a question of vaccine hesitancy. It was also a question of whether people were able to get access to the vaccine. Many people were considered essential workers, so they couldn’t easily take time off to get vaccinated. Other socio-economic factors, such as language barriers and the need for childcare, also contributed to lower vaccination rates.
“When we started our work, we didn’t want to just preach about vaccines,” Cynthia says, “We also wanted to address some of the social issues that made it difficult for people to access them.”
After receiving numerous questions about how and where to get the vaccine, the Hazels decided to partner with the Colorado Department of Public Health and Environment to host a vaccine clinic at Solid Rock Baptist Church in Aurora in February 2021. They did this with the help of volunteers through their grassroots community group called The Gyedi Project.
What started as a one-time clinic for around 50 people ended up vaccinating more than 200. They hosted three more clinics over the next three months, administering more than 2,500 vaccines in total, primarily to people of color. By June, they switched to a referral service that helped community members find vaccines at government-sponsored clinics, freeing the Hazels to shift their focus back to education.
“With the new Delta variant, we are having to step up education again, because there’s new data coming out every day and new ways of tackling the Delta variant compared to the original virus,” Kweku says.
Fears over side effects, immigration status
Fernando Holguin, MD, a professor in the Division of Pulmonary Sciences and Critical Care Medicine, is working on similar efforts to raise vaccination rates and combat misinformation in urban and rural Hispanic communities in Colorado.
“This pandemic has highlighted the tremendous social and health disparities that exist in society,” he says.
Working through the Latino Research & Policy Center (LRPC) at the Colorado School of Public Health, Holguin has been involved in weekend and holiday vaccination clinics in Hispanic communities. He also helps organize educational webinars to provide information and reassurance in a culturally sensitive, Spanish-language setting.
“It’s been a great opportunity serving the community and working with them,” Holguin says. “I’m from Mexico, so it’s a natural place for me to be.”
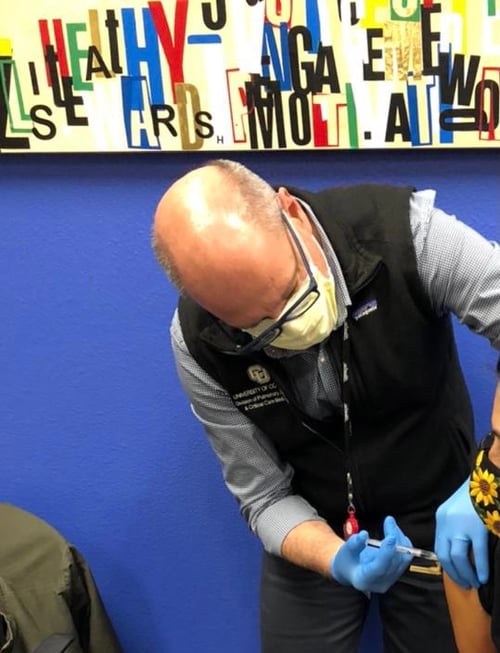
Fernando Holguin, MD, administers a COVID-19 vaccine shot at a clinic earlier this year.
From his discussions with Hispanic Coloradans, Holguin says he has learned that many are concerned about vaccine side effects and taking time off from work to get the shot. There is also fear that health care workers may be collecting information on their residency status.
“From my research, the community has been fearful for various reasons, including discrimination and the fear of deportation,” Cervantes agrees. “That’s why creating safe spaces for vaccinations has been key.”
The snowball effect and building trust
Like other providers, Holguin and his colleagues at the LRPC are finding they can increase vaccination rates most effectively by engaging trusted community officials, church leaders, and local doctors.
Another key factor in getting more people in the Hispanic community vaccinated is the snowball effect that happens when community members see friends and family members getting the shot and remaining healthy, Holguin says.
“By far the most important factor when I talk to people about why they become vaccinated is because ‘People in my house are getting vaccinated, and I see they’re doing fine,’” says Holguin.
The Hazels are taking a similar approach with their new target demographic for vaccine information: young people.
“Now that people ages 12 and up can get vaccinated, getting the youth on board is key,” Kweku says. In addition to reaching out to parents, they’ve also been training peer-to-peer youth ambassadors to connect with other young people at sporting events, music festivals, and other gathering places.
Staying ahead of the next crisis
As the pandemic continues to lurk in many communities, providers are already looking ahead to the next potential health crisis and the lessons this pandemic can teach.
The Hazels are using the increased interest to address other health issues that are prevalent within the Black community and educate people about the social determinants of health.
“When we did seminars in the past, it was difficult to get people’s attention,” Kweku says. “When COVID happened, that changed. People were now very interested in hearing about health care. So why not include information about diabetes, nutrition, exercise, hypertension, and cancer while we’re talking to them about COVID? Let’s use this opportunity to start that work right now.”
“Our communities are in this position not just because of COVID, but also because of social determinants that make us more vulnerable to a pandemic,” Cynthia says. “If there’s one positive thing that has come out of this pandemic, it’s that it shone a bright light on the fact that BIPOC [Black, Indigenous, and people of color] communities and health care providers have a lot of work to do together around community protection.”
Cervantes echoes the need to address preexisting conditions in communities of color. Recently she’s advocated for a statewide chronic kidney disease task force. Due to a higher prevalence of diabetes and kidney disease, Hispanics are at increased risk for worse outcomes from COVID-19.
Cervantes is also working with Hispanic physicians to launch the Latino Health Collaborative, a nonprofit organization that will focus on improving the health of Hispanics in the state by investing in policy development, building solidarity among Hispanic clinicians, and cultivating Hispanic clinician advocacy and health policy leadership.
“It’s my way of continuing to respond to the pandemic,” she says, “by preventing it and future pandemics from disproportionately burdening our communities.”





.png)
