A joke about bald heads by comedian and presenter Chris Rock at the Oscars ceremony last month stung patients and providers of alopecia areata (AA) around the world. Actor Will Smith’s shocking slap to Rock’s face in response ignited public awareness of a disorder that steals the hair of nearly 7 million people in the United States, many of them children.
But the emotionally challenging and disfiguring autoimmune disease that prompted actor Jada Pinkett Smith, the joke’s target, to shave her head and her husband, Will Smith, to react, has been on the radar of dermatology clinicians and researchers at the University of Colorado Anschutz Medical Campus for years.
Like many providers who care for patients who suffer from AA, Stanca Birlea, MD, PhD, was saddened by the widely publicized fiasco. “Patients with extensive or long duration alopecia areata can be severely impacted with their disease, and they need to be approached and treated with special understanding and empathy,” said Birlea, an associate professor in the Department of Dermatology at the University of Colorado School of Medicine.
For now, no cure exists, but therapy options leading to improved outcomes are expanding. Birlea and her colleagues are particularly excited about one of the latest class of drugs added to their arsenal called JAK inhibitors, she said.
Pioneering work at CU Anschutz focuses on these drugs, some given off-label to patients in its dermatology clinic and others being tested in clinical trials. All have been described as “remarkable” and “life-changing” by patients and providers.
The basics
AA, a common autoimmune disorder that affects 0.1-0.2% of the general population, causes either sudden diffuse hair loss or circular bald patches of the scalp. The condition most often targets the scalp but can cause hair loss anywhere on the body.
Over 200,000 new cases are diagnosed every year in the United States, affecting both sexes. While it can arise at any age, 80% of cases are diagnosed before age 40, with 50% of cases diagnosed in childhood. AA can have devastating consequences in all patients, but especially in children, Birlea said.

Half of alopecia areata cases strike in childhood, when school peers often lack sensitivity and tact. The emotional stress for families can be heartbreaking. |
Up to a quarter of patients have a family history of AA and/or other autoimmune diseases, with thyroid disease and vitiligo the most common. Birlea specializes in vitiligo, the disorder that caused white spots on the skin of pop legend Michael Jackson.
Atopic eczema (the most common form of eczema, which tends to run in families), is often associated with AA. AA is also prevalent in patients with Down syndrome, and faculty at the CU School of Medicine and at the Linda Crnic Institute for Down Syndrome have identified interesting clinical and molecular aspects characterizing this association, Birlea said.
Between 10% and 50% of AA patients can have nail abnormalities, including nail pitting (pinpoint depressions) and ridging (narrow raised bands) in the nail plate.
The causes
In AA, cytotoxic CD8+ T cells attack the lower segment of the hair follicles (which is called the bulb and produces the hair shaft). These T cells attack the pigment cells called melanocytes and release cytokines and chemokines, which disrupt the normal function and gradually destroy the hair follicles, Birlea said.
Genetic factors are strongly involved in the pathogenesis of AA, as suggested by heritability in first-degree relatives. Twin studies, family-based linkage studies, genome-wide association studies and candidate gene association studies have also highlighted the genetic link.
Numerous genome-wide association studies and linkage studies conducted in the last two decades have provided compelling evidence for the implication of several AA susceptibility genes, most of them with immune function, Birlea said.
Both the onset and recurrences of AA can be triggered by different factors, such as emotional stress, trauma, viral infection and hormonal changes, she said.
The effects
AA is usually asymptomatic. Some patients, however, have described burning sensation, itchiness or discomfort preceding or during the active period of hair loss, Birlea said.
The patchy AA is the most common clinical presentation. It generally affects the scalp but can affect facial hair, including beard area, and/or eyebrows and/or eyelashes. While regrowth can occur spontaneously in the bald spots, often with white hairs, new spots can appear simultaneously.
Other more severe but uncommon presentations are:
- alopecia totalis (complete or almost complete hair loss on the scalp)
- alopecia universalis (complete or almost complete hair loss on the scalp and other body areas)
- diffuse autoimmune alopecia (sudden and diffuse loss on the scalp)
- ophiasis (alopecia of back and or sides of the scalp)
Numerous lifetime recurrences are common in more than 30% of patients. Long-duration AA creates significant frustration in patients and often has mental health consequences, including loss of self-esteem, anxiety and depression, Birlea said.
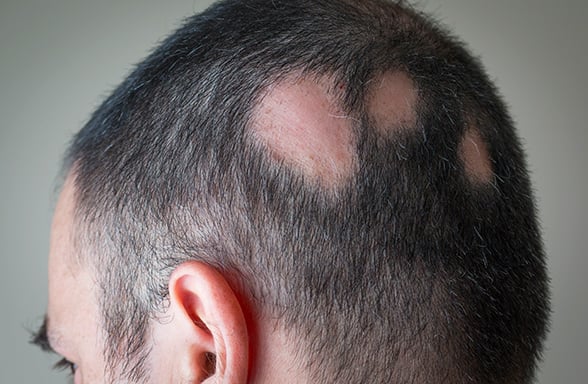
Patchy alopecia areata is the most common of the different types. The hair-loss disorder affects women and men. |
Especially in the early stages, spontaneous hair regrowth can occur, and an estimated 20% of patients can have one episode of hair loss with no recurrence during their lifetimes, Birlea said.
The therapies
No available treatments are curative. However, the hair follicle stem cell populations are preserved in AA, and hair follicles can be regenerated. Thus, hair regrowth can occur even years after total hair loss, with or without treatment.
Topical treatments include high-potency steroids with anti-inflammatory properties and Minoxidil (Rogaine) – a vasodilator with regenerative effects on the hair follicle.
Intralesional injections of corticosteroids are another popular option that can be given monthly, Birlea said. The hair regrowth effect can be temporary, however. “And the injections cannot stop onset of new bald spots in other areas, because they treat the inflammation just on the area we inject.”
Topical treatments and intralesional injections can induce hair regrowth in patchy AA or in more severe types, alone or in combination with systemic medications.
Immunotherapy uses sensitizer compounds (squaric acid dibutyl ester, diphenylcyclopropenone) that cause an allergic contact dermatitis in the lesional area. They have shown success in inducing hair regrow in patchy AA, including more extensive disease.
Providers generally reserve systemic therapy for patients with severe disease that is difficult to treat, including AA with more than 20% hair loss, rapid hair loss, chronic hair loss and/or with severe distress.
Oral steroids for short periods in combination with immunosuppressive medication given long duration (like methotrexate), are sometimes prescribed, although less so with the approval of oral JAK inhibitors, in light of their numerous side effects, Birlea said.
JAK inhibitors
Research on mouse and human hair follicles showed that topical and oral new drugs for AA – that inhibit the Janus kinase (JAK) family of enzymes, known as JAK inhibitors – reawaken the dormant follicles and prevent alopecia areata flares by blocking inflammatory signaling downstream IFN-γ and the T cell effects.
Three such JAK inhibitors already approved by the U.S. Food and Drug Administration are Jakafi®(Ruxolitinib), a medication that is used to treat bone marrow malignancies, and Olumiant® (Baricitinib) and Xelijanz®(Tofiacitinib), both medications for rheumatoid arthritis.
In a study of severe AA patients treated with oral Xelijanz for four to 24 months, 74.3% of patients showed clinical response, and 51.4% showed greater than 50% hair regrowth. “Those results could not be achieved with the standard treatments, indicating that this is a major clinical research breakthrough,” Birlea said.
“JAK inhibitors can provide excellent results, inducing significant or full hair regrowth, even in those patients who have been resistant to standard therapies or have been having long-standing disease.” – Stanca Birlea, MD, PhD
Several clinical trials are underway on JAK inhibitors, including through the dermatology department with Birlea and her alopecia areata expert colleagues: Cory A. Dunnick, MD, professor and director of clinical trials; David Norris, MD, professor and department chair; and Elizabeth Wallace, MD, assistant professor and associate director of clinical trials.
Dunnick is leading a trial of a phase 3, open-label, multicenter study looking at the long-term safety and efficacy of an oral JAK inhibitor for alopecia areata.
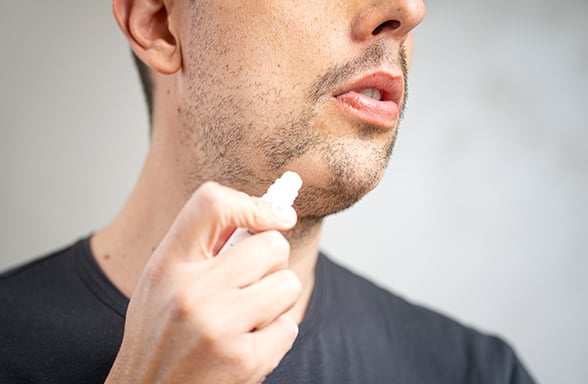
Facial hair, eyebrows and eyelashes can be targets of AA. Treatments options include topical, oral and injections. |
Dunnick, Norris and Wallace are also part of a National Institutes of Health-funded study on the use of JAK inhibitors for five skin diseases common in patients with Down syndrome (including alopecia areata) and led by Joaquin Espinosa, PhD, professor of pharmacology and executive director at the Linda Crnic Institute for Down Syndrome.
The study aims are to:
- Define the safety and efficacy of a JAK inhibitor in treating immune skin conditions.
- Reduce the burden of other autoimmune conditions more common in the Down syndrome population, such as autoimmune hypothyroidism and celiac disease.
- Explore potential benefits in terms of neurological function and quality of life.
While JAK inhibitors are promising, the treatment option is mostly symptomatic, with hair loss typically reoccurring within months of the discontinuation of therapy, Birlea said. For this reason, providers recommend it long term, trying to maintain patients on the minimum effective dose, she said.
"JAK inhibitors can provide excellent results, inducing significant or full hair regrowth, even in those patients who have been resistant to standard therapies or have been having long-standing disease,” Birlea said. “This outcome can have a profoundly positive effect on affected patients’ quality of life.”




