Editor's note: This story was reported pre-coronavirus pandemic. Educational activities are being delivered online amid the public health crisis.
It's 1:30 a.m. on Feb. 6, and the lights are bright on the fourth floor of the Education 1 Building at the University of Colorado Anschutz Medical Campus. Fourth-year medical students are interacting in an Emergency Medicine Overnight Simulation at the Center for Advancing Professional Excellence (CAPE).
In one bed, a patient is suffering from a ruptured ectopic pregnancy. Next door, a patient is suffering from sepsis due to a urinary tract infection, and the final room holds an intoxicated and combative patient.
This isn't the first overnight emergency medicine simulation, but it's one to remember. Events cascade at a rate similar to a busy hospital, with students being pushed to manage an assortment of problems, further enhancing real-life scenarios.
Innovation through collaboration
For over a decade, the collaboration between CAPE and the Department of Emergency Medicine has been nothing short of innovative. To leverage this relationship and prepare CU students for residencies in Emergency Medicine, Assistant Professor Mike Overbeck, MD, created the Emergency Medicine Boot Camp.
It’s a two-week capstone course designed to provide students with confidence and subject-matter competence as they transition to emergency medicine residencies. The offering of transition courses to prepare students in specific specialty subject matter has been increasing nationally.
Pre-pandemic, Dr. Mike Overbeck briefs the simulation staff before the overnight session.
"The key event in the curriculum is an immersive, high-fidelity, 15-hour simulation event that takes place overnight,” Overbeck said. “In this simulation, learners gain exposure to a wide variety of stressors, including simulation scenarios of shock, altered mental status, consent, decision-making capacity and acute agitation. Transitions of care, including sign-outs at the beginning and end of the experience, bookend this on-call experience. Phone calls covering common cross-cover questions, the performance of procedures, and bedside ultrasound imaging are spread throughout the session."
Gaining confidence before residency
The goal: for students pursuing emergency medicine to gain exposure and confidence before heading to residency. Unlike similar offerings across the nation, this is the only course to simulate an overnight call while requiring students to actually participate overnight.
Overbeck said, "Our motto is 'Competence with Confidence.' The duration and overnight aspect of the simulation adds a dimension of fatigue and stress inoculation that shorter sim events cannot replicate. That realism is essential when we try to impart confidence in our learners. In the end, we want them to say, 'No matter how tired or cognitively overloaded I feel right now, I can do this.'”
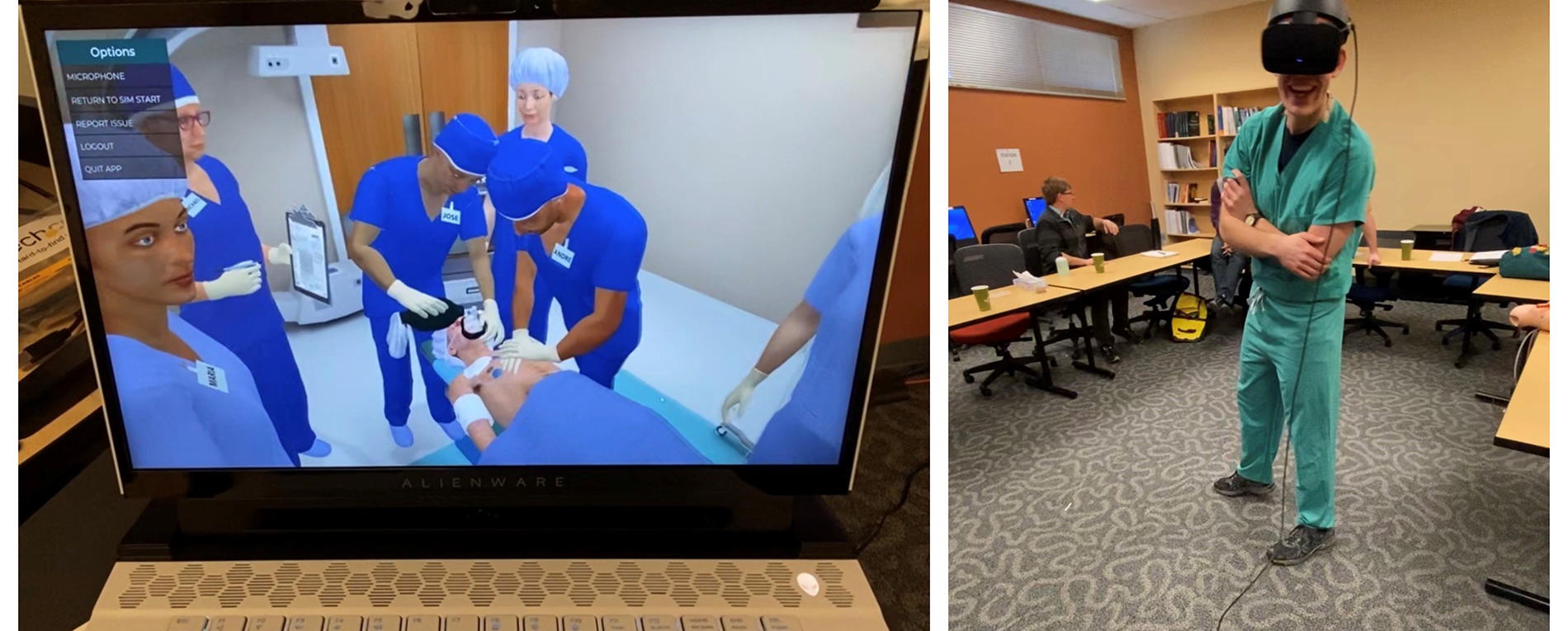
Nearing the end of this arduous overnight journey, students also navigate a virtual reality Advanced Cardiac Life Support (ACLS) "megacode."
"Introducing the ACLS VR simulation was an exciting way to find where virtual reality fits in with our curriculum,” said Brian Kelly, simulation education specialist. “The simulation allowed our students to experience rapid-fire ACLS algorithm training during a limited-rest situation without having to pull other healthcare professionals in for assistance.
Adding virtual reality to the mix
Kelly noted that virtual reality is becoming another tool to use in simulation exercises. “The intention isn't to replace real-life simulations any more than mannequins intend to replace real-life patients,” he said. “Finding the niche that virtual reality fits in will open up a wide range of possibilities that will allow us to cultivate even better healthcare providers."
For the learners, it was an invaluable experience. Ryan Hirata said the ACLS VR sim forced him to apply his knowledge and confront his deficiencies. "It is effortless to pick a multiple-choice answer or draw a diagram for ACLS algorithms. When you see a rhythm change on the monitor and need to react immediately, you have to know ACLS. The VR did a great job of showcasing the difference between book knowledge and its application.
The VR simulation highlighted any weaknesses on a score screen, allowing students to improve their performance in real time.
“I enjoyed the sense of stress/urgency the virtual reality provided and am very appreciative that I could make the mistakes caused by that sense of stress in a sim rather than in real life," he said.
Importance of communication
Hirata said the VR sim also drove home the importance of communication. “Having the VR force me to say, 'Phyllis, defibrillate the patient at 200J' is excellent training for a stressful environment where direct, detailed, and concise communication is vital to prevent confusion and patient harm."
This ambitious undertaking requires commitment from a sizeable group of CAPE experts to support the authentic learning environment. Devra Keyes, a simulation technician and simulated patient, said, "The learners were required to deal with ill patients, upset family members and over-worked staff, which required everyone to think on their feet in the wee hours of the morning."
That's why places like CAPE exist – so learners have a safe place to practice their skills. CAPE continues to grow and innovate while bringing world-class education to current and future professionals in the Denver metro area, the region and beyond.
Guest contributor: Jocelyn Blake, simulation education project coordinator, Center for Advancing Professional Excellence (CAPE)