If the first century of the University of Colorado College of Nursing is known for its growth and dedication to educate students and care for patients, CU Nursing may be remembered in the last 25 years of its history for focusing on the individual. In the last quarter of a century, faculty have innovated new programs to serve and meet the unique needs of the diverse, Indigenous, uninsured and rural patient. In the middle of this fine-tuning of accessible healthcare came a big wrench. COVID-19.
The pandemic stopped the progress and faculty had to pivot and learn how to adapt in a new world where everyone was afraid to get sick or already infected, and nurses quit in droves to protect themselves and their families. But lest we get ahead of ourselves, let’s go back a quarter century when faculty were pioneering new ways to serve.
Family Health

Sheridan Health Services |
In 1995, the Sheridan School District started a school-based health center with Children’s Hospital and pediatric nurse practitioners from the College of Nursing. Midwifery care was also launched for students and women in the community.
With grant funding from the U.S. Department of Health and Human Services, Health Resources and Services Administration, CU Nursing took over the project in 2005 and called it Sheridan Health Services (SHS). Amy Barton, PhD, RN, FAAN, ANEF created the vision and strategic initiatives for SHS. A subsequent grant application in 2010 led to awarding of federally-qualified health center status in 2012.
The nonprofit federally-qualified community health center is run by advanced practice nurses. Today, SHS is recognized as an exemplary nurse-managed community health center with the ability to provide high quality, compassionate care.
SHS serves a pocket of poverty where 90% of the children have free or reduced lunch. The clinics are located in medically underserved, low socioeconomic urban areas in Arapahoe, Jefferson and Denver counties. Sixty-eight percent of the population is Hispanic and Latino, and half don’t speak English. The SHS staff can communicate with its 4,175 patients in their own languages during 16,300 clinical visits a year.
It also provides education for nursing students. In 2022, 102 nursing, behavioral health, dental and pharmacy students performed more than 13,000 clinical hours at SHS.
SHS has three locations serving adults and children: The CU Family Health Clinic, CU Belleview Point Health Clinic, and the CU Youth Health Clinic which is school-based. Today, a multidisciplinary team composed of nurse practitioners, doctors, registered nurses, public health nurses, dentists, hygienists, pharmacists, behavioral health providers and support staff provide integrated services.
“Having school-based health centers are extremely important for education, access to care, and developing trusting relationships to face life’s stressors,” says Erica Sherer, DNP, MSN, BSN, RN and SHS CEO.
“We provide comprehensive, culturally-responsive care with a focus on wellness and disease prevention to help patients, regardless of their ability to pay.”
The community health center has been critical to the population as Hispanic residents are 20% more likely than whites to die of treatable conditions such as asthma attacks, diabetes complications, appendicitis, and certain cancers.
SHS has established a substance use treatment program for patients including pregnant women, and recently launched a refugee program. Nurses and pharmacists work under a Collaborative Drug Therapy Management program to optimize drug therapy and lifestyle modification for patients which has led to dosage reductions and deprescribing of medications while improving chronic care outcomes for those with hypertension, diabetes, and dyslipidemia.
SHS has strong roots within the communities they serve including formal agreements with Swedish Medical Center, University of Colorado Hospital, Littleton Adventist Hospital and Children’s Hospital Colorado to ensure smooth transitions of care for patients.
Delivering local care
In the future, SHS plans to hire staff to serve more patients, deliver more local care with mobile units, and help close the digital divide with telemedicine. The pandemic accelerated the need for telehealth across the board. SHS wants to reach the most vulnerable clients without access to the internet.
In 2022, 89% of its patients using telecare were white and spoke English. Denver’s most vulnerable are already feeling severe economic and health impacts from the COVID-19 crisis, and they are further at risk of being left behind now that health care, education and other social services require people to have stable digital access.
The plan is to provide physical equipment like vital sign displays, blood pressure cuffs and pulse oximeters along with hot spots to partnering organizations like Urban Peak as they did in the Arapahoe Library District during the pandemic to promote health equity and digital literacy.
Practicing what they preach
Beginning in the late 1990s and through today, one big factor set CU Nursing faculty apart from many other nursing colleges. They teach and work. Former Associate Professor Sue Hagedorn, PhD, RN, helped set the bar for teachers to practice what they preach.
“We just went out and found sites for faculty to practice. We found help was needed everywhere in residential treatment centers, high schools, even in the prison system for juveniles and women. Everyone at the time needed a part-time nurse practitioner. So, we marketed ourselves and ended up with a huge faculty practice,” says Hagedorn, retired from the University of Colorado College of Nursing.
“Now all faculty are strongly encouraged to practice. It gave our students an experience and best practices from their faculty. It made all of the difference.”
Hagedorn, who produces documentaries today, also directed a mentoring program for middle school students when she was faculty. Partnership in Prevention was a long-term mentoring program for at-risk adolescents. She also established other faculty practices for at-risk and underserved populations.
“We had alcohol and drug abuse prevention money from the state, so we provided experiences for faculty and staff to mentor students. We also had graduate nursing students take courses about preventing domestic violence,” Hagedorn says.
Online Learning
In 1997, CU Nursing made it possible for graduate students around the world to get a top-ranked education with a 100% online Master of Science in health care informatics. This innovative program was led by professor emeriti Diane Skiba, PhD, FAAN, FACMI who is known internationally as a pioneer in nursing informatics. The infrastructure established and the success of the program led to the creation of a second online degree program in nursing leadership, i-LEAD or Innovation in Leadership and Administration in Nursing and Health Care Systems. The web-based program guides nurses into leadership and administrative responsibilities in primary care, long-term care, home health positions and more.
In 2023, US News & World Report ranked i-LEAD as 11th best online leadership program in the country out of 200 programs. The program is taught by professional educators who are also nurses and researchers. The goal is to foster nursing leadership and reduce health disparities. i-LEAD is one of 12 master’s degrees offered by the college.

Fitzsimons Army Medical Center in 1973 |
The Big Move
Today, the University of Colorado Anschutz Medical Campus is the largest academic health center in the Rocky Mountain region. That happened in 2004 after six health sciences-related schools and colleges including the University of Colorado School of Nursing moved to the Fitzsimons campus and was renamed the College of Nursing in 2008. The University of Colorado Hospital, Children’s Hospital Colorado and the Rocky Mountain Regional Veterans Affairs hospital also moved to the campus.
The grounds used to be part of the Fitzsimons Army Medical Center, which was decommissioned by Congress in 1999. In 2006, the Anschutz family donated $91 million and the campus became their namesake. Together, the organizations improve the quality of patient care, research and education.
Midwifery Care
Building on more than 20 years of providing midwifery care to women without insurance and those with Medicaid at UCH, CU Nursing conceived the Center for Midwifery model at the Anschutz Medical Campus in 2004. The concierge perinatal practice was established by Erica Sherer in conjunction with Amy Barton. The center offers comprehensive services with a focus on the family’s physical and emotional needs. The model has been replicated under the leadership of Jessica Anderson to two communities in Lone Tree and Longmont. Today, there are four nurse-midwifery faculty practices in Colorado which partner with local hospitals and offer clinical experience for master’s and doctoral students.
Director Jessica Anderson says her dream is to offer more midwifery services statewide, particularly in rural areas where health care access is lacking.
“Our future goals are to provide access to nurse midwifery care in communities that don’t have it. That’s why we started practices in Lone Tree, Longmont and Highlands Ranch hospitals. Our goal is to expand, serve more patients and create additional clinical experiences for our students,” says Jessica Anderson, DNP, CNM, WHNP, FACNM, Midwifery Services director.
Another reason for Anderson’s push to expand midwifery services is the perinatal morbidity and mortality rates in the United States. It has the highest rate among 11 developed countries worldwide. Federal data shows the nation’s maternal death rate rose significantly in 2021, with the rates among Black women more than twice as high as those of white women.
Anderson says midwifery has favorable outcomes and a specific philosophy of care that is focused on meeting the needs of the individual.
“Midwives tend to utilize fewer interventions, improve outcomes and have higher patient satisfaction. Yet, midwifery is underutilized in the United States. Midwives work in health care teams where we consult with our physician colleagues as needed,” says Anderson.
“People should have access to all maternity care providers, philosophies, and access to evidence-based care to have the best outcomes and experiences possible.”
On the Anschutz campus, it’s the best of both worlds. We collaborate with providers from different disciplines and nursing to provide the best care to our patients. At AMC, our university nurse-midwives practices staff the Obstetric Emergency Department (OB ED) service. Pregnant and postpartum patients are first evaluated by a midwife in the OB ED. Patients are admitted with the service they received prenatal care from or with our physician colleagues if a high-risk condition is identified.
“The collaboration with medicine is important to the success of our program. It combines the best of both worlds. Having a strong, trusting collaboration relationship with OB-GYN is important and has improved astronomically over the last several decades,” says Anderson.
About 150 babies every month are delivered across the midwifery practices.
“The reason midwifery has expanded and become popular is for choice and movement and for birth to be approached as a natural life event rather than a medical condition. It’s a philosophy about midwives meeting the needs of people by being present and providing emotional support and coaching. In other words, letting nature take its course and intervening only if necessary,” says Sherer.
In 2022, the American Academy of Nursing designated CU Nursing Center for Midwifery as an Edge Runner; a nurse-designed, innovative models of care or interventions with significant, demonstrated outcomes to improve health, impact cost and influence policy. Each of these programs highlights nurses’ ingenuity and collaboration in developing new methods to provide care and promote health equity.
Student-Run Clinics
CU Nursing Midwifery practices also have a clinic at Anschutz that is run by a midwife and learners including medial students and advanced practice nursing students. The midwife supports the learners and patients in the clinical setting. It’s a great approach to interdisciplinary learning and collaboration.
The Summit Virtual Prenatal Program
The CU Midwifery faculty practice also launched virtual prenatal care in 2023. Patients receive almost half of their prenatal visits right in their home. It combines in-person and virtual visits during the pregnancy and postpartum periods. Patients are provided a baby doppler, blood pressure monitor and a scale so they can complete components of the visit at home.
“We connect with patients virtually and conduct the visit by videp. We ask patients typical questions just like an in-person visit, and the patient conducts the hands-on portion of the visit like listening to the baby’s heartbeat, checking their blood pressure, and their weight.
“This is one of our solutions to access care in rural areas. Even in the Denver Metro Area, some people’s travel time is significant and a barrier to keep their appointments, or they might have to drive 70 minutes to get access to prenatal care. We’re trying to be thoughtful and creative about care delivery for people in those situations,” says Anderson.
Peer Support Doula Program
The Peer Support Doula program also launched in 2023 to support patients with a history of substance use disorder through pregnancy, labor and birth, and one year postpartum with a peer support specialist trained as a doula. Among other things, the doula offers patients emotional and physical support before and after pregnancy and education and support.
“In Colorado, the top two killers of mothers who are pregnant and postpartum are suicide and accidental drug overdose. This program aims to provide patients with substance abuse disorders additional support. This program doesn’t exist anywhere else in Colorado and we’re proud to offer it to our parents,” says Anderson.
Working Together
In 2010, CU Nursing collaborated with academic leaders across campus to create an experience for students from all professions to learn and work together to solve medical problems. It’s called the Center for Interprofessional Practice and Education (IPE). In classrooms, teams of nursing, dentistry, pharmacy and primary care students communicate, collaborate and solve problems. It’s a reminder to each student they’re just one piece of the puzzle, which ultimately makes them better clinicians.
“The Interprofessional Practice and Education program on the Anschutz Medical Campus is one of the leaders across the country. Often times students might learn about some of these skills within their own curriculum but they never really get a chance to practice that in a team environment and that’s where the IPE curriculum really propels our students ahead of others,” says Amy Barton, a member of the inaugural team.
CU Nursing also established a presence at the Dawn Clinic, an IPE student-run free clinic that delivers primary care to uninsured people in Aurora. It gives the IPE students from Anschutz an opportunity to take care of actual patients, be in the community and work together.
Switzerland Ties
In 2019, CU Nursing made history by pioneering a program with Bern University of Applied Sciences in Switzerland. Nurses here are teaching Swiss nurses advanced practice nursing skills to meet a critical shortage of healthcare professionals facing an aging, sicker population in the west European country.
The program was created by Kelly Stamp, PhD, NP-C, RN, CHFN, FAHA, FAAN, associate dean of Academic Programs, and associate professor after she learned about the shortage of general practitioners in rural areas.
“These advanced nurse practitioners can be based in the rural health system in the mountains, help with primary care, help with access to care, and help those who really can’t afford a lot of care,” says Dr. Stamp.
“The role of nurse practitioners is not in competition with physicians in Switzerland, it is in complement with physicians. Just like in the United States, we're not trying to be physicians, we're trying to improve patient outcomes and complement the role.”
Pivoting in the Pandemic
In March 2020, COVID-19 forced university students around the country to quarantine at home and learn online. That was a disaster for healthcare students who could no longer practice in clinics and earn the hours required to graduate. Faculty at the CU Nursing had to pivot.
They expanded simulation training for students to practice with lifelike mannequins (also known as mannikins), virtual reality, task trainers, and other methods to complete their clinical rotations and earn their degrees. As a result, CU Nursing was the first and only department on the Anschutz Medical Campus to return to in-person learning during the pandemic.
The high-quality simulation education was a success. The director of the Clinical Education Center and Simulation Fara Bowler, DNP, APRN, CHSE says the students graduated with the same state board exam pass rates as previous graduating classes. A study by the National Council State Board of Nursing also found simulation learning was equal, if not better, than learning in some clinical situations.
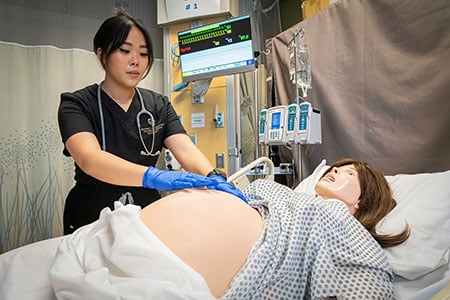
CU Nursing student practice skills on pregnant manikin |
In 2023, CU Nursing expanded simulation space by 15,000 square feet. The additions at Anschutz Medical Campus, the Legacy Innovation Campus and Fort Lewis College will create the largest nursing simulation space in the Rocky Mountain region, 20,401 square feet, by 2024.
“We are moving nursing education forward for our college through advancements in technology and other learning innovations,” says CU Nursing Dean Elias Provencio-Vasquez, PhD, RN, FAAN, FAANP.
COVID-19 also caused other changes. People learned the importance of hand hygiene, self-care and staying home when sick. However, the epidemic was grueling for nurses.
“Nurses went from already having full workloads to working six days a week, scrambling to care for people remotely without the technology in place, and testing people for the virus,” says Sherer.
“We were the first university to get the testing kits and we also worked with the state to open vaccine clinics for patients. But nurses got burned out. While other people were working from home, we still had to manage our families and jobs,” recalls Sherer.
Future Voices
In June of 2020, after news about the murder of Minneapolis resident Geroge Floyd and police shooting Black Americans, Omarah Macias and other students at CU Nursing started the student organization Future Voices to help foster diversity, equity and inclusion. Their goal is to take collective action against racism and prevent social injustice while changing the ethnic makeup of nursing. In 2023, 66% of registered nurses are white and 88% are women.
Future Voices mentors high school students about the nursing profession. The group of undergraduate and grad students also helped induct Zipporah Parks Hammond, the first Black nurse who graduated from the University of Colorado School of Nursing in 1946, into the Colorado Women’s Hall of Fame.
In 2022, CU Nursing named Emily Gamm, MSW to the role of DEI coordinator. Her job is to cultivate nurses who reflect various communities and are culturally responsive to provide compassionate, person-centered care.
The college also showed its commitment to creating a diverse student population with its Integrated Nursing Pathway (INP) program that paves the way for students at three local community colleges to transfer to CU Nursing. Students in the INP program account for 72% of students at the college from underrepresented populations.
A Four-Corners Workforce
In 2022, CU Nursing teamed up with Fort Lewis College (FLC) in southwestern Colorado to build a nursing workforce of rural, Indigenous and tribal students. The collaborative is the first of its kind in Colorado and will provide innovative solutions to nursing shortages in rural areas, health inequities in diverse communities, and diversification in the profession. FLC has a high diversity rate with almost half of its student population Native American and Alaska Native.
The first cohort of students arrive in the fall of 2023 to study pre-requisite courses in science and liberal arts taught by FLC faculty. In summer 2025, 24 students will be admitted to the nursing major and receive instruction from CU Anschutz nursing faculty for the final two years of their four-year degree.
Graduates will earn a bachelor of science degree. The program and its offerings are unique in the US.
Amy Barton helped develop the partnership and funding. Barton is the professor and senior associate dean for faculty and students at CU Nursing at the Anschutz Medical Campus and is also the Daniel and Janet Mordecai endowed chair in rural health nursing.
“Indigenous people are grossly underrepresented in the health profession. So, this is an excellent opportunity to bring a high-quality education program to them in their community. This collaborative is an innovative solution to nursing shortages in rural areas, health inequities in diverse communities and shows how colleges can work together to provide better healthcare,” says Barton.
The program will experiment with new approaches to rural nursing education, including designing simulation labs that incorporate Indigenous healing, creating communities of practice that connect regional health practitioners, and bringing together telehealth with culturally responsive care.
Closing the Gaps
In May of 2023, CU Nursing partnered with six states to create the Clinical Nursing Faculty and Preceptor Academy (CFPA) for the Rocky Mountain region. The program, led by Montana State University, provides training and tools to strengthen and support clinical nursing faculty and preceptors working in rural and frontier parts of the mountain west.
The partnership includes the Montana Office of Rural Health/AHEC, the Colorado Center for Nursing Excellence, and Colleges of Nursing at the University of Colorado, Montana State University, North Dakota State University, South Dakota State University, Utah, and Wyoming.
Teams made up of people from the six states will create and implement curriculum to prepare existing professional nurses to teach other nursing students and enlarge the nursing workforce. The four-year project will train and support 900 clinical faculty and preceptors, especially in the nation’s poorest rural areas where there is limited access and large disparities in healthcare services.
The maternal mortality rate in rural areas is almost twice as high than in urban settings, partly because there is a workforce shortage, according to a study by Jessica Anderson and Amy Barton in 2021.
“I think it takes a special person to live and work in rural areas as a nurse. We want to educate people there who we know will want to remain in their community with the right resources and practice,” says Barton
AI and new technology
Like every aspect of life, artificial intelligence (AI) is offering many benefits to the nursing profession. AI technologies are providing tools and systems to assist patient care and identify patterns and trends to make more accurate diagnoses and treatment decisions. AI-powered devices and sensors are monitoring patients remotely and collecting real-time data on vital signs, medical adherence and other indicators. The technology is also being used in education with realistic simulations and scenarios for students to practice their skills, enhance critical thinking and prepare nurses for real-world patient care situations.
In August 2023, two CU Nursing professors held a pilot study to test how smart glasses can help students during medical exercises. Professors could talk to and guide students who were wearing the smart glasses with a microphone while they performed CPR on high-definition mannikins in the college’s simulation lab.
“(The technology) can help patient outcomes, enhance nursing training, and give information to nurses who don’t have certain training,” says Senior Director of the Experimental Learning Team Fara Bowler, DNP, APRN, CHSE.
“This study hopes to use the research to improve student learning in controlled environments, advance nursing education, and expand the roles of nurses.”
The Future
Leadership is already working hard to diversify the workforce, make healthcare more accessible to people in rural and impoverished areas with more telehealth, and mentor preceptors to attract new talent into the profession.
But by all accounts, the pandemic changed health care and the profession is still adapting.
Jessica Anderson believes the future needs to include innovative care-delivery models and programs to meet people where they are and fill the gaps.
Amy Barton sees a positive future as the college continues to innovate with nurse-led models of care. She expects online education to grow, students and nurses to have more flexible schedules and, with focus, patients to have equitable health care.
“CU Nursing has an amazing foundation. We’ve benefited from many visionary leaders and we’ve been able to do things in Colorado that may not necessarily have happened in other places. Given the amazing human capital that our faculty bring, I think our future is nothing but bright,” says Barton.
Sue Hagedorn says future education will depend upon how health professionals integrate themselves in the community and connect with people either online or in person. She’s an advocate of nurse theorist Jean Watson’s Theory of Human Caring, which includes showing patients you’re present, committed to their care, and involve them in their own healthcare. To end the nursing shortage, Hagedorn believes students will have to find meaning in their work to make it through future problems and pandemics.
Erica Sherer strives to improve health equity and reduce health related disparities in the future by expanding integrated care across Colorado through strategically-aligned partnerships. She will also continue to work on reducing the digital divide with more access to telehealth. Her goals will take a team of future interprofessionals to provide comprehensive care and find solutions to serve patients no matter who they are, how much money they have or where they live in Colorado.
National Recognition
The University of Colorado College of Nursing at the Anschutz Medical Campus has received multiple awards in the last 25 years including:
- Best Masters in Nursing and Doctor of Nursing Practice Programs in Colorado and the nation - U.S. News & World Report (2023)
- Top 10 Best Nursing Schools in Colorado - Nurse.org (2022)
- Top 10 Best Online Nursing Programs and Top 11 for Leadership Programs in the U.S. – U.S. News & World Report (January 2023)
- Top Masters and DNP programs – U.S. News & World Report (April 2023)



