What is the treatment for gliomas and other cancers that start in the brain?
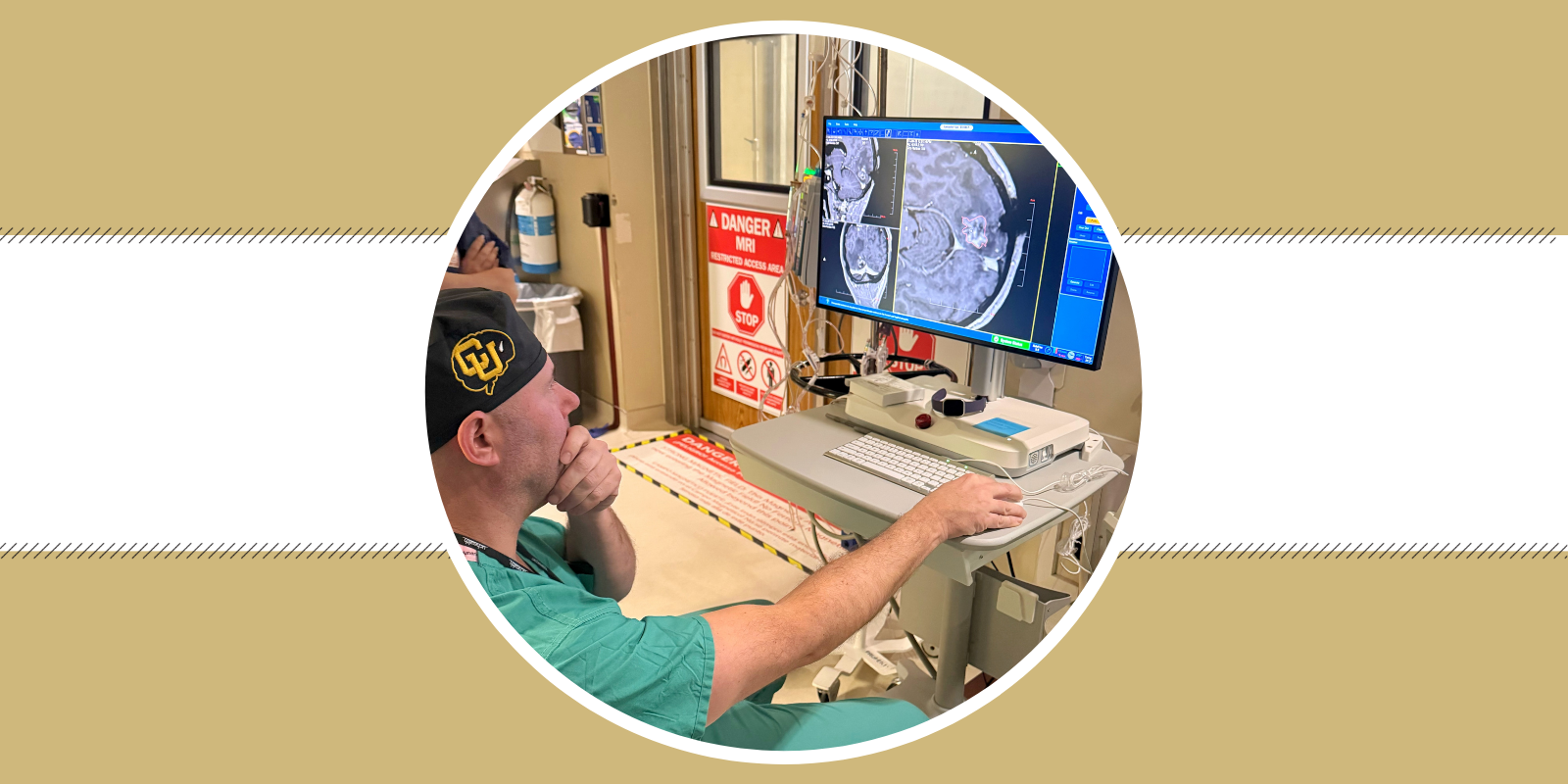
The first thing we have to decide, when we look at these tumors, is if they can be surgically removed. If we don't think we can get at least 90% of it safely, we tend not to remove it. If we do think we can get 90% of it safely, we'll offer a surgery, and then, in the weeks after surgery, primary brain tumors will be treated with a combination of a drug called temozolomide, which is an oral chemotherapy agent, and usually about six weeks of radiation.
That radiation is called EBRT, or external beam radiation therapy, and people usually get it five days a week for six weeks. It takes a couple of hours a day. It's done on an outpatient basis, but it's a long regimen. It has to treat the whole tumor and surrounding areas in the brain.
After that, people will then go on what's called metronomic temozolomide, which means they're only on it for about one week out of each month.
>> Learn about glioblastomas.
By contrast, what is the treatment for other cancers that spread to the brain?
Brain metastases are very different. The typical cancers that a brain metastasis would come from are lung cancer, breast cancer, and melanoma, but there are less common ones, like gastrointestinal and genitourinary cancers.
All of those cancers have different chemotherapies that are being used to treat them — melanoma has different drugs than lung cancer, which has different drugs than breast cancer. When people develop brain metastases, they're still going to be on some type of systemic agent that treats the primary cancer; however, if someone develops brain metastases while on one of those therapies, we often consider them to have failed that therapy. The medical oncologist may switch out agents at that point and switch to one that has better penetration into the brain.
Most brain metastases will also get a specific type of radiation called stereotactic radiosurgery, or SRS, which is radiation that is surgically precise to just target the lesion itself. Unlike patients with glioma, who inevitably will fail radiation and at some point recur, radiation for brain metastases in the form of SRS has about 85% to 90% local control rates. Sometimes we can eliminate brain metastases just with stereotactic radiosurgery.
Is surgery typically done on cancers that spread to the brain?
In a glioma case, you need a surgery to reduce the size of the disease so there's less for the radiation to act on. That's what we do with surgery for brain metastases as well. But we will generally operate on only one or two brain metastases, even if there are more present. Usually the ones undergoing surgery are larger and more symptomatic. If they're larger than two to three centimeters and causing problems, we want to get them out so that the SRS has a better chance of being effective and to alleviate the symptoms that the lesions are causing. If someone has 20 brain metastases and they're all small, we're not going to go in and take any of those out, but patients will get radiation to all of them.
The therapies we have for brain metastases are more effective, so the role of surgery for brain metastases is defined, but less frequent. For primary brain tumors, we want to offer surgery to everybody we can; with metastases, it's reserved for large or symptomatic lesions, and that’s followed by a focused beam of radiation that is generally delivered in one to five doses, instead of the 30 doses that primary brain tumors most typically get.
Is immunotherapy used to treat either type of cancer in the brain?
There are no FDA-approved immunotherapies for primary brain tumors, but there are a variety of systemic cancers that go to the brain in which immunotherapy, particularly in the form of a drug called checkpoint blockade, like nivolumab or pembrolizumab, can be quite effective, particularly for melanoma. They are so effective now that sometimes we don't need to give radiation for melanoma that metastasizes to the brain; we can just give immunotherapy and then wait and see. Unfortunately, those same drugs have not shown a lot of efficacy against primary brain tumors.
Whether they are primary brain tumors or metastases, have these cancers become more treatable over the years?
When I started my training some 20 years ago, we would often tell people with brain metastases from melanoma that they had something like three to six months to live. And now, we talk about cures. We didn't operate on metastases as much back then, because those cases were thought to be hopeless in some ways. Now, we very firmly understand the role of surgery, and we have much more effective therapies, allowing us to be more aggressive with brain metastases. For gliomas, the therapies haven't changed that much in the past 20 years. There are a lot of people, including myself and my lab, who are looking to find ways to make immunotherapy work better in glioma.
The largest advance in the past few years is for lower-grade gliomas that have a mutation in a gene called IDH1. There is now a drug called vorasidenib that targets that mutation. The phase III trials were just published in December of 2025, and there appears to be some promising efficacy there.
May is Brain Cancer Awareness Month; what is most important for people to know about brain cancer?
I think our therapies are getting better and more well tolerated. There are outdated notions of people becoming super sick from their therapies, of radiation knocking people down for a while, or of brain surgery potentially being unsafe. We can do things much more safely now, through much smaller incisions, and the role of surgery has increased as we've developed more tools to allow us to operate in parts of the brain that previously we thought weren't safe.
The big message, I would say, is don't give up, and don't presume that brain cancers are a death sentence. That's just not true. Seek treatment. But be aware that all of the really excellent treatment options are more so going to be available at academic centers. I frequently get patients who say, “I was told this was inoperable,” or, “There was nothing they could do,” and then, years later, they're thankful that they came to us and we were able to offer them something that many patients or providers may not have even know existed. My biggest piece of advice is to get yourself to an academic center like University of Colorado.