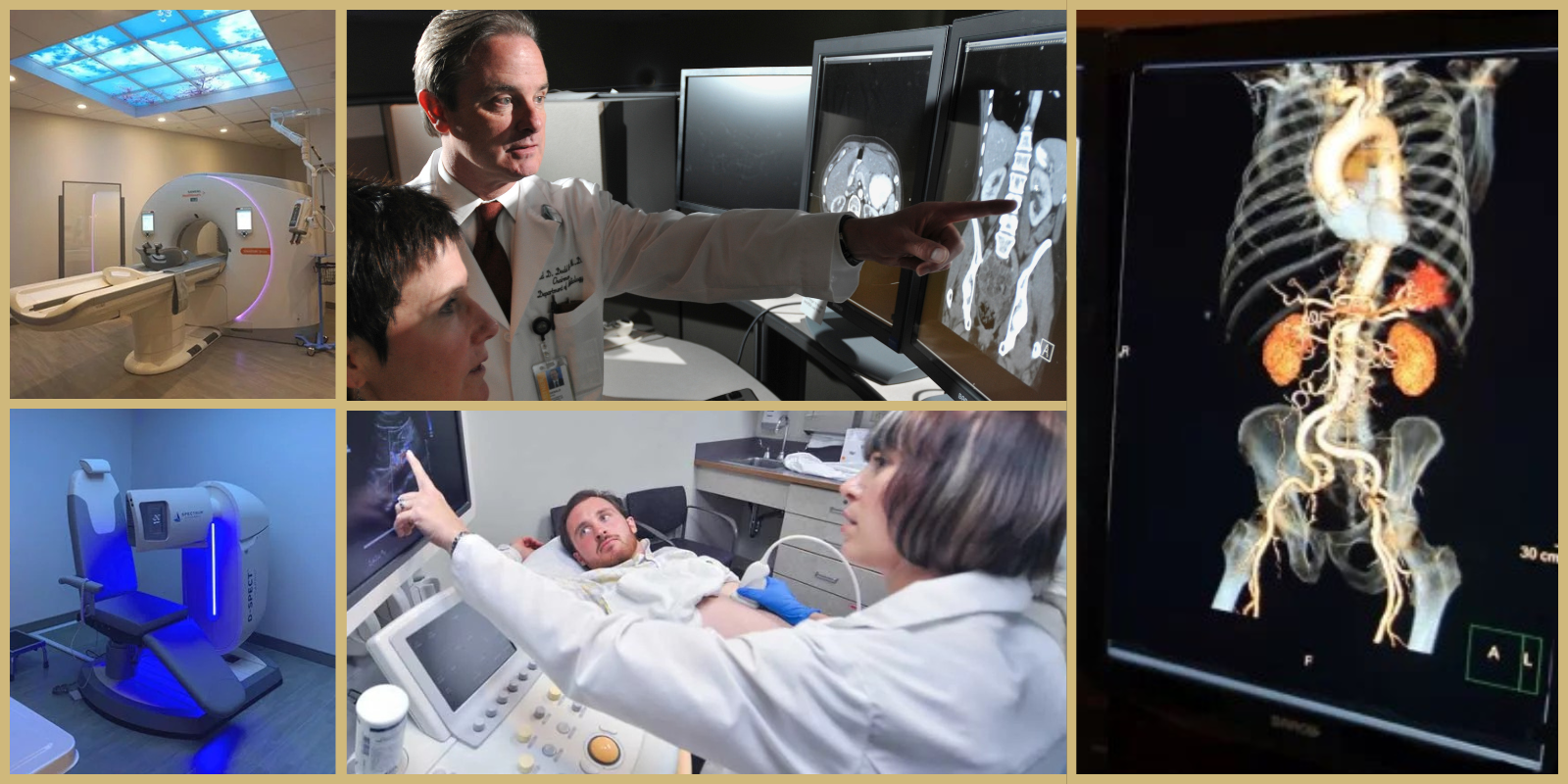
Put in the most basic terms, medical imaging means “using different techniques to non-invasively try to figure out what’s going on with somebody,” says University of Colorado Anschutz Cancer Center member Dulcy Wolverton, MD.
Across a career spanning more than three decades, Wolverton – an associate professor and section chief of breast imaging in the CU Anschutz Department of Radiology – has seen those techniques grow ever more sophisticated, from rows of x-rays on plastic film to the computer-processed 3D digital imagery of today.
“As we become more able to do different kinds of imaging, we get finer and finer detail,” Wolverton says. “Advances in imaging have given everyone in medicine more information than we ever had before.”
During Wolverton’s fellowship in the early 1990s, if a doctor suspected breast cancer in a patient, “that meant a diagnostic surgical biopsy,” she says. “Women were having a lot of surgery. And we didn’t have breast surgeons, just general surgeons. There was an awful lot of maiming – just terrible, disfiguring surgeries. And in general, only 30% to 40% of those surgical biopsies found cancer.”
Later, with the advent of mammography and ultrasound imaging to guide needle biopsies that were far less invasive than surgery, “that changed everything,” she says.
In the cancer realm, providers now have an arsenal of imaging tools at the ready, not only to detect cancer, but also to assess how far the disease has spread, target treatment while reducing harm to patients, and evaluate treatment success. These tools involve x-rays and other forms of radiation as well as sound waves, magnetic fields, and radio waves to create images with the aid of powerful computers.
As imaging has advanced, the role of radiologists – doctors who specialize in medical imaging – has expanded in cancer care, Wolverton says.
“Originally we were consultants to the clinicians who were seeing patients and didn’t necessarily see the patients ourselves. Now, increasingly, we’re very involved with patient care. Often we’re the ones who find the cancer. At the CU Anschutz Cancer Center, we’re part of the multidisciplinary clinic for each patient, along with surgeons, medical and radiation oncologists, pathologists, and many others.”
But the sheer variety of these imaging tools – MRI, CT, PET, x-ray, mammography, ultrasound, and more – can be bewildering to many of us. What are they? How do they work? What are they used for? For answers, we turned to Wolverton. Here she explains several imaging technologies most commonly used for cancer.
X-ray
It’s ionizing radiation passing through a part of the body that’s being imaged. It’s usually low dose so it doesn’t cause harm. The x-rays used to expose film on the other side of the object, but now they create images on a digital detector. It can give you an overview of whatever object stops the x-ray beam, like a bone or a large tumor, but it doesn’t look inside an object.
Mammography
It’s used for screening for breast cancer and also for diagnostic purposes. It’s a very high resolution x-ray taken of breast tissue. It can see calcifications – hardening of tissues from calcium buildup – that are less than a millimeter in size that could be a sign of the earliest changes that can turn into breast cancer. We get very valuable information from mammography on calcifications that isn’t revealed in other methods.
Now, instead of just a 2D mammogram, we’re doing an upgrade called digital breast tomosynthesis, where we take multiple images through the breast that can be reconstructed into 3D slices. That allows us to see through dense breast tissue that could be masking cancers.
Ultrasound
Ultrasound doesn’t involve radiation. It’s a beam of high-frequency sound waves sent from a transducer to scan though an object and see soft tissues in real time. The beam bounces off objects and sends back echoes that tell us something about what we’re seeing – is this something benign, or something more typical of cancer? Those two will look very different. If we put together an x-ray and an ultrasound, that gives us a better sense of the whole object we’re looking at.
MRI (magnetic resonance imaging)
This gives you a very, very detailed view that’s really amazing. A magnetic field applied to the body aligns protons in the body’s water molecules to the direction of the field. And then a radio frequency pulse is applied to knock the protons out of alignment. When the pulse stops, the protons spin back into alignment, and the machine measures differences in how quickly they spin back to create an image showing you differences between various types of tissue. It gives you an anatomical image from the inside.
MRI shows you slices through a body in whatever orientation you want, and you can get a nice overview of an object by stacking the slices.
You can add a contrasting agent, called gadolinium, intravenously. It’ll flow through the blood vessels, so you can see the vessels, see tumors that are getting a lot of blood, and see where the tumors are in relation to surrounding structures.
MRIs are super-useful for finding breast cancer, but we also use them a lot for cancer staging – determining how much cancer is in the body, where it’s located, and how much it has spread. An MRI also might be useful if you’re worried that there’s brain cancer.
CT scan (computer tomography)
This is a kind of x-ray, again, but it gives you more information. This time you’re getting a full 360-degree view to show a cross-sectional slice of the body. CT is widely used for detection of cancer and for staging. You might have a chest x-ray and see something in a lobe of the lungs, and the CT scan can give you more detailed information – is it lung cancer? How much is there? For staging you can see what lymph nodes are involved with the cancer.
Bone scan
It’s a technique that uses nuclear imaging to detect bone diseases, including cancer. It uses a small amount of injected radioactive tracer material – usually Technetium-99m – that will bind to some part of the body you’re interested in, such as bone tissue. More of the radioactive material collects in areas where there’s extra metabolic activity going on, such as a tumor.
Then the patient lies down on an exam table and a gamma camera passes over the body, building an image that shows spots where there’s extra radioactivity. It’s useful for detecting cancers that have metastasized to the bone from other areas, which is part of the staging that will influence treatment decisions.
PET scan (positron emission tomography)
This is a nuclear medicine technique as well, but it uses a different radioactive tracer, called fluorodeoxyglucose (FDG), attached to a sugar analog that will be taken up by any metabolically active part of the body. It’s taken up especially rapidly by cancers, which are usually more metabolically active than most of the body. The patient goes through a rotating scanner, and the image shows bright spots where the metastases are. It’s usually layered on top of a CT scan to produce 3D images with anatomical information.