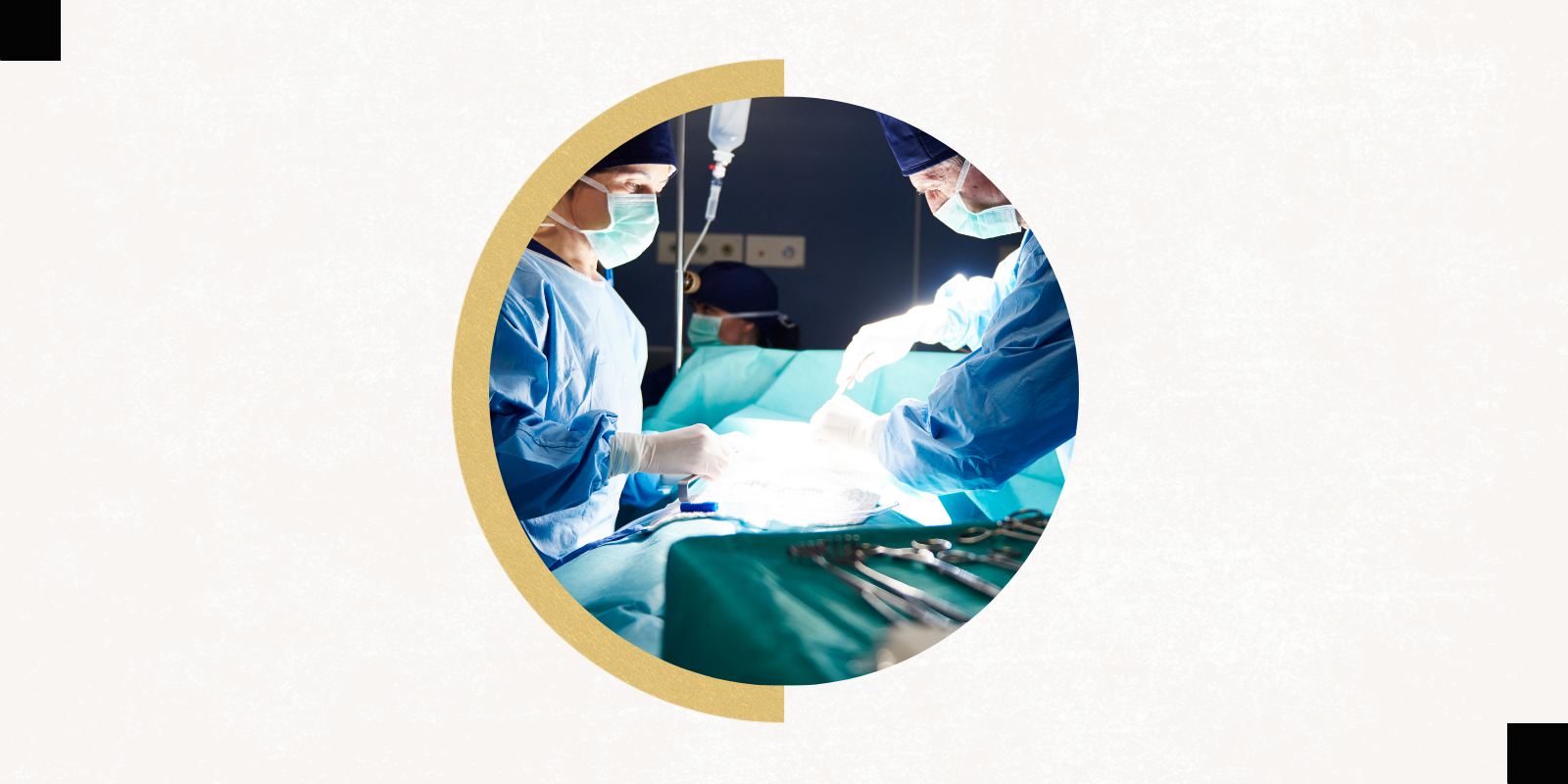
At first, she was reluctant to talk about it – a little sheepish, even. The obvious question was, “Why are you doing this?” And though she had answers, none of them were quick or easy.
The simplest explanation that Rachel Davis, MD, associate professor of psychiatry in the University of Colorado (CU) School of Medicine and vice chair of Clinical Affairs, could give for donating more than 50% of her liver to a stranger is that she wanted to and she was able to.
“I don’t feel comfortable with this donation being portrayed as selfless or heroic,” Davis says. “While donating part of my liver offered me no medical or physical benefit, the experience has provided immense psychological and even spiritual benefit.”
Today, on Donate Life Living Donor Day and more than two months since her surgery, Davis has grown increasingly comfortable talking about her living donation journey as a way to “normalize the experience and the option of living donation,” she says. “I’m no longer embarrassed, and it no longer feels like bragging to talk about it. It just feels meaningful and exciting, and it’s not something that needs to be hidden.”
Taking risks that align with her values
Davis, who grew up on the plains of eastern Colorado, has always been motivated to work hard and excel in everything she did. She knew from a young age that she wanted to be a doctor and determinedly pursued a path to medical school.

Rachel Davis, MD, began working as an EMT at age 16
It was during her medical studies that she first learned about living organ donation, and, “I remember thinking, ‘I need to do this’,” Davis says. At the time, nondirected living donation, or donation in which the organ does not have an intended recipient, wasn’t common or really even discussed.
Despite her desire to donate, the demands of medical school couldn’t accommodate a commitment as significant as living organ donation. But it was something Davis always kept in the back of her mind.
“I’m not a thrill seeker or adrenaline junkie, but I have taken a number of risks throughout the course of my life, all in line with my values and sense of purpose in life,” she explains. These have included working in a Mozambique orphanage shortly after the civil war there ended and traveling through Madagascar when the country was experiencing plague outbreaks.
So, when she came across an article on the UCHealth website about a nondirected living organ donor, she decided it was time to seriously pursue the thing she’d been thinking about for years.
Moving forward with a longtime thought
As Davis began moving forward on the path of nondirected living organ donation, she did worry whether her mental health diagnoses, which include obsessive-compulsive disorder (OCD), would limit her ability to donate. She has always been very open about her diagnoses to help combat stigma and show that physicians can have mental illness, receive treatment, and have successful careers. However, she wasn't sure whether her mental health diagnoses would preclude her from going any further in the donation process.
“But the transplant team didn’t just say no,” she says. “I knew I was going out on a limb filling out the initial medical history form, and I was prepared to be dismissed – I would have been disappointed but not devastated or humiliated. But they didn’t dismiss me. Instead, they were realistic about the potential concerns associated with my psychiatric diagnoses and thoughtful about my life context. They were non-judgmental and compassionate.”
Still, as the possibility of nondirected living organ donation became more of a reality, Davis hesitated to tell people. What would they think? That she was doing it for selfish reasons, for the attention or accolades? She cringed at the thought, and at first only told her younger sister, who lives in Durango, but not her parents; her sister told them.
“I emailed them when I knew I was actually going forward with it, and they said they were dismayed at first because I’m their daughter and they worry, but now that I was going forward with it they were very proud of me,” Davis recalls.
As a medical doctor she was very aware of the risks involved, but as a psychiatrist she also was aware of the psychological, mental, and emotional ramifications of what she was considering.
“I would say I’m a very empathetic person, and in trying to understand myself, why maybe I was doing this, I was reading some of the literature about altruism and empathy,” she says. “I also treat patients with OCD, and it’s just fascinating to me that the pathway we stimulate with electricity in deep-brain stimulation is the part of the same brain circuitry that’s activated when people engage in compassionate behaviors.”
The activation of this pathway, which is involved in producing rewarding feelings, balances out the pain that highly empathetic people experience when they perceive the suffering in the world around them.
“People who are highly empathetic but feel helpless and don’t do something about what they see, all the pain in this world, are at increased risk for burnout and compassion fatigue,” Davis explains. “When you can do something about the suffering, life in this world becomes more tenable.”
An unexpected meeting with her recipient
Several months ago, Davis received the go-ahead to become a nondirected living organ donor. Though she felt a bit of guilt stepping away from not only her responsibilities to her patients, but her various leadership responsibilities in the CU School of Medicine Department of Psychiatry during the height of the Omicron COVID-19 surge, “so many people offered to cover my patients and cover my roles,” Davis says. “I have amazing and generous colleagues.”
Two days of tests and evaluations preceded the actual surgery, and on January 19 transplant surgeon Elizabeth Pomfret, MD, PhD, professor and chief of transplant surgery in the CU Department of Surgery, removed the right lobe of Davis’ liver – about 55% of the organ.
"A nondirected anonymous donor is always extraordinary," Pomfret says. "Especially for a physician to do this and take time off from their practice speaks volumes about the kind of selfless person she is. The selfless nature of people who are willing to donate a part of themselves to someone they don't know is always extraordinary.”
With her mother, sister, and good friend helping her through six days of recovery in the hospital and then recovery at home, Davis journeyed through moments of significant pain and adaptation. She knew that within the first two months most of her liver would regenerate.
As she recovered, she had time for reflection. Even though the understanding in nondirected living donation is that the organ will go to a stranger whom the donor may never meet, Davis wrote a brief note to her recipient and left it with Pomfret to pass along. In the note, she simply wrote that she was glad she was able to make the donation and she hoped the recipient was doing well.
Not expecting to hear anything in return, she received an email from Manny Ortiz, whose wife, Lety, was the liver recipient. The New Mexico couple were still in Denver and wanted to meet Davis.
“That’s not something I necessarily expected to happen, because I would imagine for some recipients it would be weird to have this person in your life, not knowing whether you want to manage a relationship like that,” Davis says. “But they asked to meet, and they’re both just beautiful people. We talked for a long time, and Lety even made me soup.”
Lety Ortiz told Davis that as her liver was failing and she was at her sickest, an angel came to her in a dream and told her everything would be OK and she would receive a liver. She had that dream the same month that Davis began the evaluation process for donation.
Normalizing the experience of living organ donation
Now, Davis considers the lengthy scar that bisects her abdomen a badge of honor. She has a number of tattoos on her torso and back symbolizing her various travels and life experiences, “and this is a version of a tattoo, except with even more meaning,” she says.
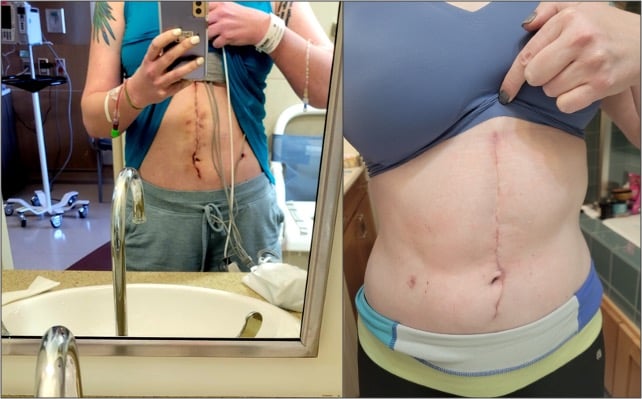
Rachel Davis, MD, considers the scar that now bisects her torso a badge of honor
She is less apprehensive about discussing her experiences with nondirected living organ donation and wants to destigmatize a process that some might hesitate to undertake because the worry that others will think they’re doing it for attention or accolades.
“I recognize that my ability to donate comes from a place of privilege,” Davis says. “I’m privileged in health, both physically and mentally. I'm privileged financially in my ability to afford taking time off work. I’m privileged to have family, friends, and coworkers who supported me through this process.”
The journey of living organ donation allowed her to push past significant fears – fear of death, fear of how others might perceive her – and gain increased empathy for her patients who struggle with chronic illness.
“My body survived more than 50% of my liver being removed,” Davis says. “My body is strong and remarkable. While it’s important to acknowledge that living donation is a significant endeavor with real risks, I also want to normalize and demystify living donation for others who may be considering it. This has been a life-changing experience.”