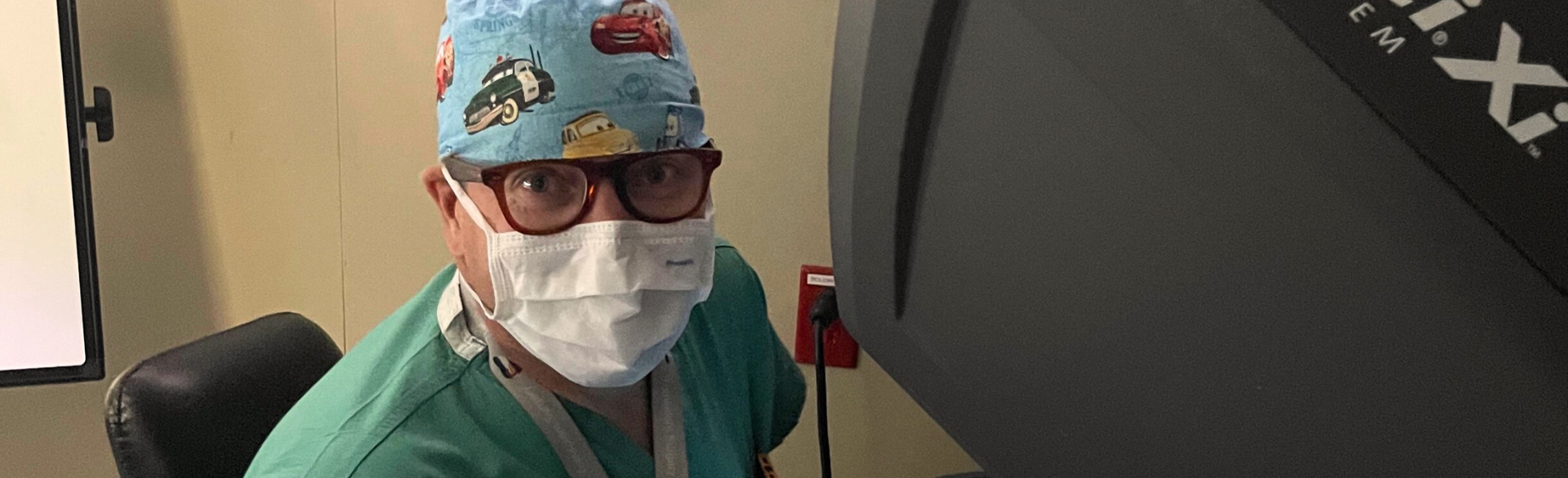
Aiming to increase the number of living liver donors by making liver donation surgery easier and quicker to recover from, the University of Colorado Department of Surgery recently performed its first robotic hepatectomy (surgery to remove a portion of the liver) from a living donor. Using a surgical robot to perform the procedure results in a smaller incision, less scarring, less pain, and a faster recovery for the donor.
“There are a lot of advantages to using the robot for this operation,” says Trevor Nydam, MD, associate professor of transplant surgery, who led the team that performed the first robotic surgery at CU. “Once you get through the learning curve and you're able to fully use the robot, the visualization is excellent. The technique allows us to be gentle with the tissue. Our hope is that it helps to remove some of the disincentive to donation, getting people back to work sooner. They don't have to take as much time away from their normal daily life to recover from this.”
The in-hospital stay for a traditional open hepatectomy is typically five to seven days, Nydam says; with robotic surgery that time is reduced to two to three days. Patients can return to normal life in three to four weeks after robotic surgery, versus the eight weeks it takes after traditional open surgery.
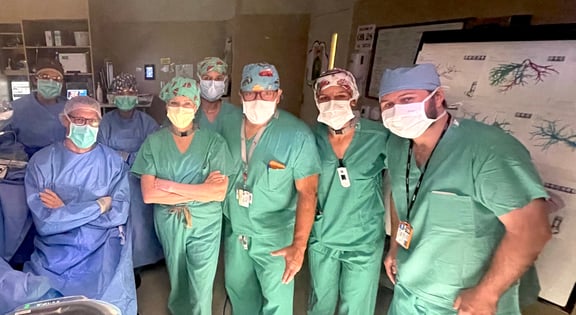 Nydam and his team after performing their first robotic liver transplant.
Nydam and his team after performing their first robotic liver transplant.
A boon for parent donors
Although the first robotic hepatectomy performed by CU surgeons involved a nondirected donor — or an altruistic donor who doesn’t know the recipient of their donation — using the robot for surgery also is an advantage in situations where a child is in need of a liver transplant and a parent wants to be the donor, Nydam says.
“That's very important so they can get back to taking care of the child who just had the transplant,” he says. “We don't want the donor who might be a parent to be out of the game on taking care of their child after they get a transplant. There are a lot of advantages to this approach, if we can move it forward and do it in a safe way.”
High-volume training
Nydam received the bulk of his training on the surgical robotic procedure in Saudi Arabia, where religious and cultural customs have resulted in most organ donations coming from living donors. Surgeons there have worked for years to perfect a robotic procedure that makes people more likely to donate, and Nydam was grateful to receive the benefit of their knowledge.
“We were poised to be in a good position to go there and learn from those surgeons and bring the technique back to CU,” Nydam says. “We feel very comfortable offering it to our potential donors. In the future, this is the way the operation is going to be done.”
The future of living-donor liver transplants
The recipient surgery is not done using a robot, Nydam says, though that technique is beginning to be studied at other surgery centers around the country. The primary advantage is for the donor, as he saw in Saudi Arabia, where surgeons are able to perform several such surgeries a week. And while deceased donors still play a large part in the liver donations that take place in the U.S., he sees the use of the robot as the beginning of a shift to using more living donors whenever possible.
“For us, it's about finding the right recipients to get living donors, and then making sure that we give any potential donors the opportunity to donate to their recipient,” he says. “It is important that we maintain a culture in which living donation becomes a primary means to get somebody transplanted. It’s an option we need to look at early. It shouldn’t just be a backup if you can't get a deceased donor.”
The first robotic hepatectomy in the CU Department of Surgery, which took place in June, points to the success the program hopes to have going forward. The donor was in the hospital recovering for half the time it takes to recover from traditional open surgery, Nydam says, and she had no complications. It’s a hopeful sign at a time when the need for liver donors is higher than ever.
“It’s well known that there are a lot of people waiting for a transplant. We have a lot of people on the list, and the donor gap continues to be significant,” he says. “It’s important to do anything we can to increase the frequency of living donation.”
Lead photo: Trevor Nydam, MD, behind the controls of the surgical robot.