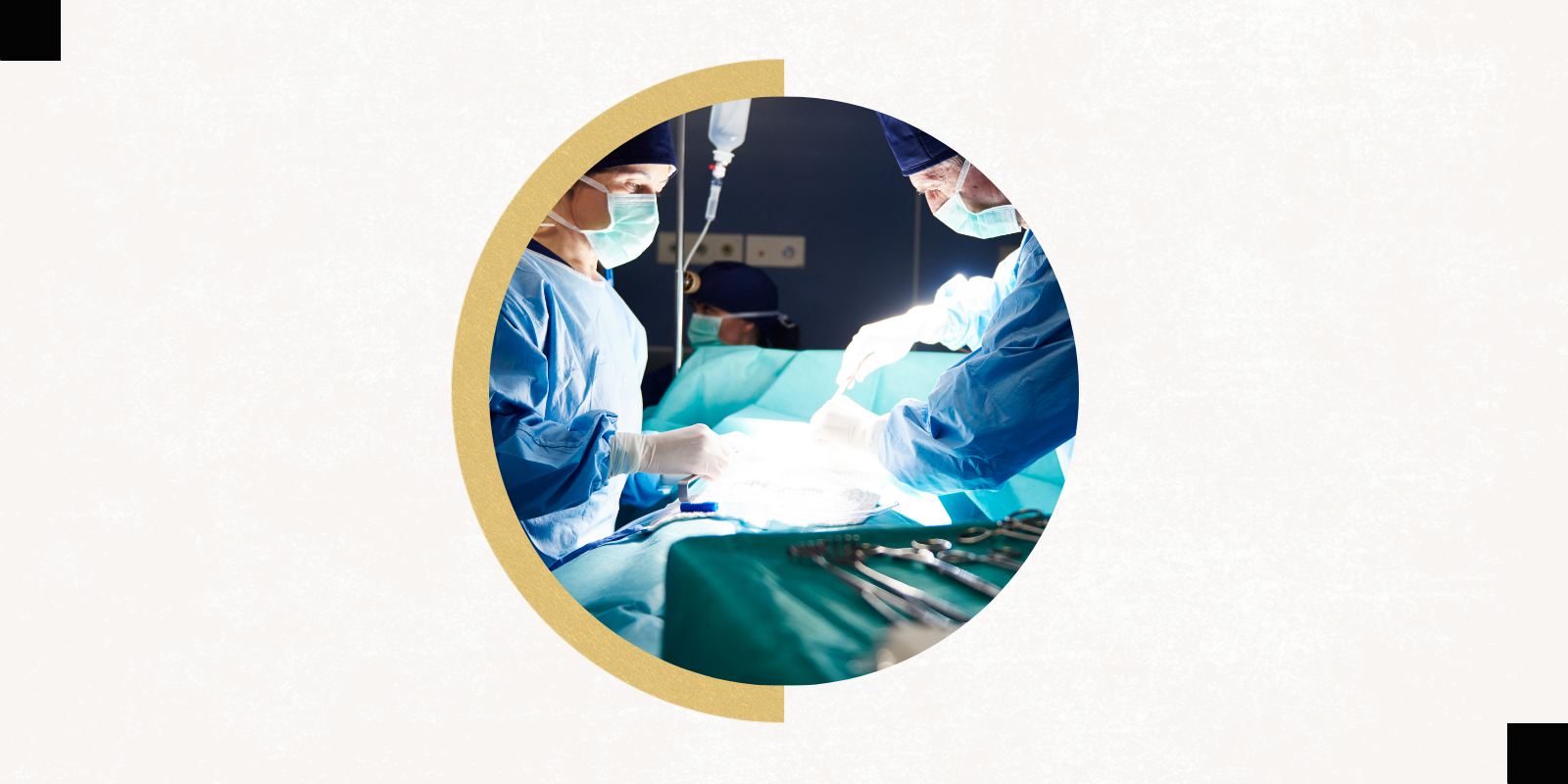
Even before the robot, the University of Colorado Department of Surgery was leading the way when it comes to mitral valve surgery. Morbidity and mortality outcomes for mitral valve repair at CU are well below the national average. In 2019, CU surgeons began using a minimally invasive approach to repair leaky heart valves that affect blood flow in the body and can lead to congestive heart failure.
“Guidelines support repairing — rather than replacing — mitral valves when possible,” says Jessica Rove, MD, associate professor of cardiothoracic surgery. “We know that mitral valve repair is very successful in helping patients avoid the sequelae of severe mitral regurgitation including dilation of the heart chambers, atrial fibrillation, and heart failure.”
The minimally invasive approach involves going between the ribs on the right side of the body to operate on the heart. Surgeons don’t have to break the breastbone or any other bones, giving patients a quicker and potentially easier recovery.
Enter the robot
In 2022, Rove and Joseph Cleveland, MD, chief of cardiothoracic surgery, began looking to improve patient outcomes even more. Rove trained in the use of a surgical robot to allow her greater precision when performing the operation. She and her team traveled to several sites around the country and trained for months to gain proficiency in the technology-aided technique.
“With the robot, you can drive the camera into the heart and get a 3D, high-definition view of the valve,” she says. “It’s a level of detail that you could never get traditionally, even wearing loupes. Additionally, your robotic instruments have a greater range of motion than the human hand, and your instruments are inside the heart. You are essentially doing the procedure with your hands inside the heart.”
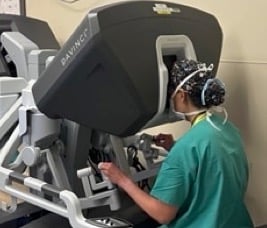 Jessica Rove, MD, at the controls of the surgical robot.
Jessica Rove, MD, at the controls of the surgical robot.
Rove and her team performed their first robotic procedure in February 2023 and have done 12 more since. Efficiency has improved, she says, and the results have been great. The robotic procedure has also meant a reduced length of stay in the hospital after surgery — from an average of 6.8 days to 3.8.
Easier recovery
Additional advantages of minimally invasive robotic surgery, as opposed to a traditional sternotomy, include less blood transfusion, easier wound healing, and fewer restrictions after the procedure.
“We have no activity restrictions after the robot-assisted, minimally invasive mitral surgery, because you’re not breaking any bones,” Rove says. “If you have a sternotomy, you can’t lift more than 10 pounds for four weeks; you can’t drive a car for four weeks. With the minimally invasive procedure, I had one patient who was playing tennis a month after surgery. That doesn’t happen after a sternotomy.”
Patient perspective
One of the first patients to undergo the robotic procedure was Jeannie McNeilly, of Denver, who had a robotic mitral repair in February 2023.
“At my first appointment, I was favorably impressed by Dr. Rove as she stared at the computer screen showing my faulty mitral valve,” McNeilly says. “I could see it in her eyes that she was thinking, ‘I know what I’m going to do when I get in there.’ I could see the wheels turning.”
McNeilly had almost no pain after her procedure, and she was up and walking the same day as her surgery. She left the hospital after three days and did the rest of her recovery at home.
“Dr. Rove was clearly a skilled surgeon intent on solving a serious problem in the best way possible,” McNeilly says. “I resolved to put my heart health in her hands, and I haven’t looked back.”
Uniting a team
Robotic mitral valve surgery doesn’t just have advantages for patients, Rove says; it also presents a greater collaborative opportunity for the surgical team. While Rove sits behind the controls of the robot, other highly trained specialists are at the patient’s bedside, assisting and managing the robot. For Rove, that team includes Meredith Stasi, PAC, Tamara Mayne, RN, Ronny LaMar, RN, Joe Morabito, DO, with cardiac anesthesia, Michelle Benson, and George Justison with perfusion.
“With traditional heart surgery, the surgeon controls a lot at the bedside,” says Rove, who did her surgical residency at the CU Department of Surgery and became the department’s first female attending cardiothoracic surgeon in the CU Department of Surgery when she returned in 2018 after a fellowship at Washington University in St. Louis.
“When you expand to using the robot for cardiac surgery, you are dependent on a team of people, and everybody has to speak up,” Rove continues. “We had to feel very comfortable communicating as a team, and that changes the dynamic in the operating room. We put a lot of trust in each other. It has really elevated the game of some of the people involved in the operating room, and it’s really highlighted some of the skills of other people on our team, which has been very fulfilling to see.”
The time spent training on the surgical robot has more than paid off, Rove says, and the improvement it makes in patient outcomes has made robotic surgery her new standard of care.
“With the robot, we can inspect the valve with really nice detail and figure out exactly where we think the areas are that need to be addressed,” she says. “The repairs are great — they look fantastic, and most importantly, our patients are doing well. We are so pleased to now be able to offer this to our patients.”