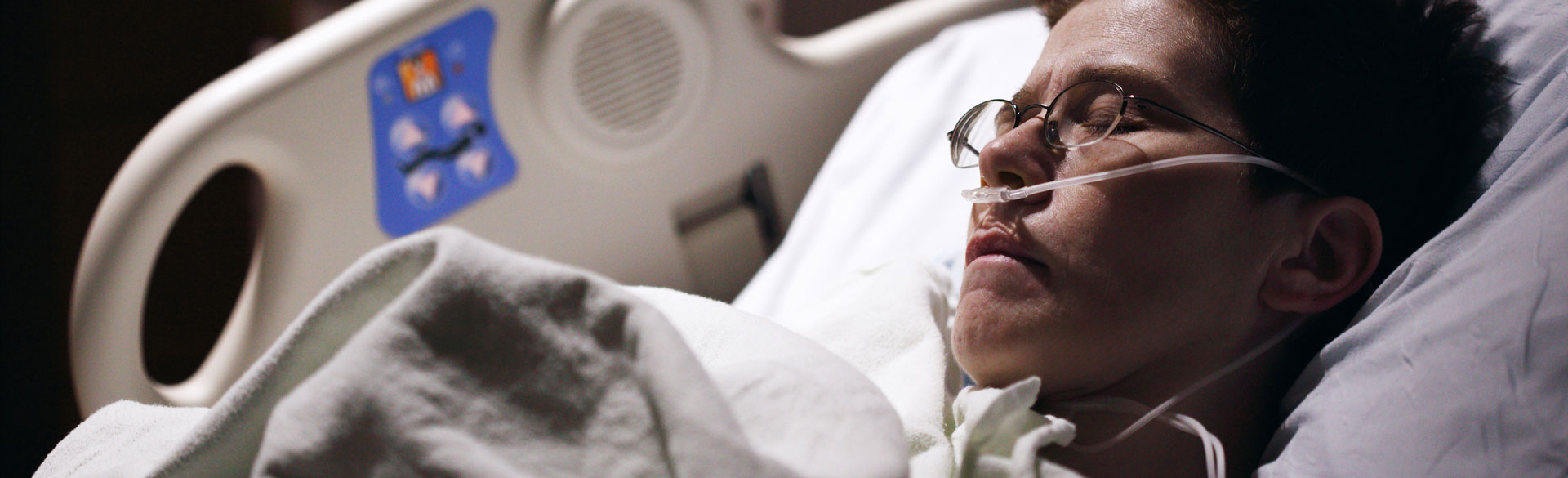
When John was in the hospital last month getting ready to have open heart surgery, he felt exhausted. It wasn’t just from his damaged heart. John couldn’t get enough sleep. As soon as he dozed off in the evenings, at least three medical professionals woke him up to take blood, deliver medicine and ask questions. John wondered why they couldn’t all come at once and let him get some rest. As it turns out, he’s not alone in that idea.
New research shows 50% of all acutely ill patients have their sleep disrupted in hospitals. That deprivation can slow down their recovery and increase the risk of falls, delirium and death.
“When patients are in critical care and don’t get quality sleep, they may not enter the REM cycle, which is required for a true state of sleep, relaxation and restoration,” said the authors of an evidence-based practice initiative, Brian A. Rottweiler, MS 2020, RN and Mary Beth Flynn Makic,PhD.,RN.
“The more often patients are woken at night, the less time they will experience deep restorative sleep, which can impact their sleep-wake cycles or circadian rhythm, and ultimately, their health.”
The evidence-based practice initiative was implemented by an Adult-Gerontology CNS graduate of the University of Colorado College of Nursing and was published in the Journal of PeriAnesthesia Nursing.
The main causes of sleep disruption and delirium are noise, lighting and nursing care, according to the paper. The Society of Critical Care Medicine (SCCM) says those issues can be fixed with simple measures and a coordinated effort.
SCCM guidelines call for clinicians to give patients earplugs and eye masks, and teach them about the importance of sleep. Studies show earplugs and eye masks alone increase quality sleep and reduce the risk of delirium.
Guidelines also call for hospital personnel to keep patients awake during the day by opening the window blinds and turning on the lights to suppress melatonin and by keeping patients alert and engaged. Without that, critically ill patients will sleep during the day –up to 57% of their total sleep time, which makes it harder for them to sleep at night and feel fully rested and restored.
At night, hospital personnel should keep the lights off, blinds down and make the patient care area as quiet as possible. Research by the World Health Organization shows noise levels over 40 to 55 dB will cause adverse health effects and wake people up.
Also, clinicians should make it a goal to wake patients as few times as possible during the night so patients can fall into a deep sleep and achieve a full sleep cycle, which takes on average 90 to 120 minutes.
Despite growing evidence about the imperative need for quality sleep, studies show only 8% of healthcare personnel believe prioritizing it is important. In addition to delirium, not getting enough of and the right kind of sleep can adversely affect patients’ glucose regulation, immune response and blood pressure regulation.